
Intrapersonal communication is the conversation you have with yourself. It includes thoughts, self talk, reflection, memories, values and the way you interpret what is happening around you. When you pause before speaking, question your reaction or replay an event in your head, that is intrapersonal communication.
It often goes unnoticed because nobody else can hear it. Still, it affects how you speak, how you listen and how you respond under pressure. In health and social care, that private thinking can shape tone of voice, patience, body language and judgement in very visible ways. A helpful overview of communication in care can be found in the Skills for Care communication resources.
A worker might meet a person who is distressed, frightened, withdrawn or angry. The spoken words are only one part of that exchange. The worker’s inner response often sets the direction. A thought such as, “Slow down. They may be frightened, not refusing”, can change the whole interaction.
“What staff say to themselves often shapes what the person receiving care experiences.”
This is more than general thinking. It usually involves several mental steps at once. A person may notice an emotional reaction, question an assumption, reflect on past experience and choose a calmer response. That inner process supports safer communication and steadier care.
It also affects people receiving support. Someone living with pain, disability, anxiety or loss may have a harsh inner voice that tells them they are a burden or that nobody will listen. Those thoughts can reduce confidence and make it harder to ask for help. The Mind information on self esteem is useful here because it shows how private beliefs can shape behaviour.
A simple way to think about it is this. Intrapersonal communication is the private conversation behind public behaviour. In care settings, it can support empathy, reflection and professionalism. It can also create problems when it becomes rushed, negative or based on poor assumptions. That is why it deserves close attention.
Useful background can also be found in NICE guidance on patient experience, NICE guidance on shared decision making and NHS England’s work on communication with patients.
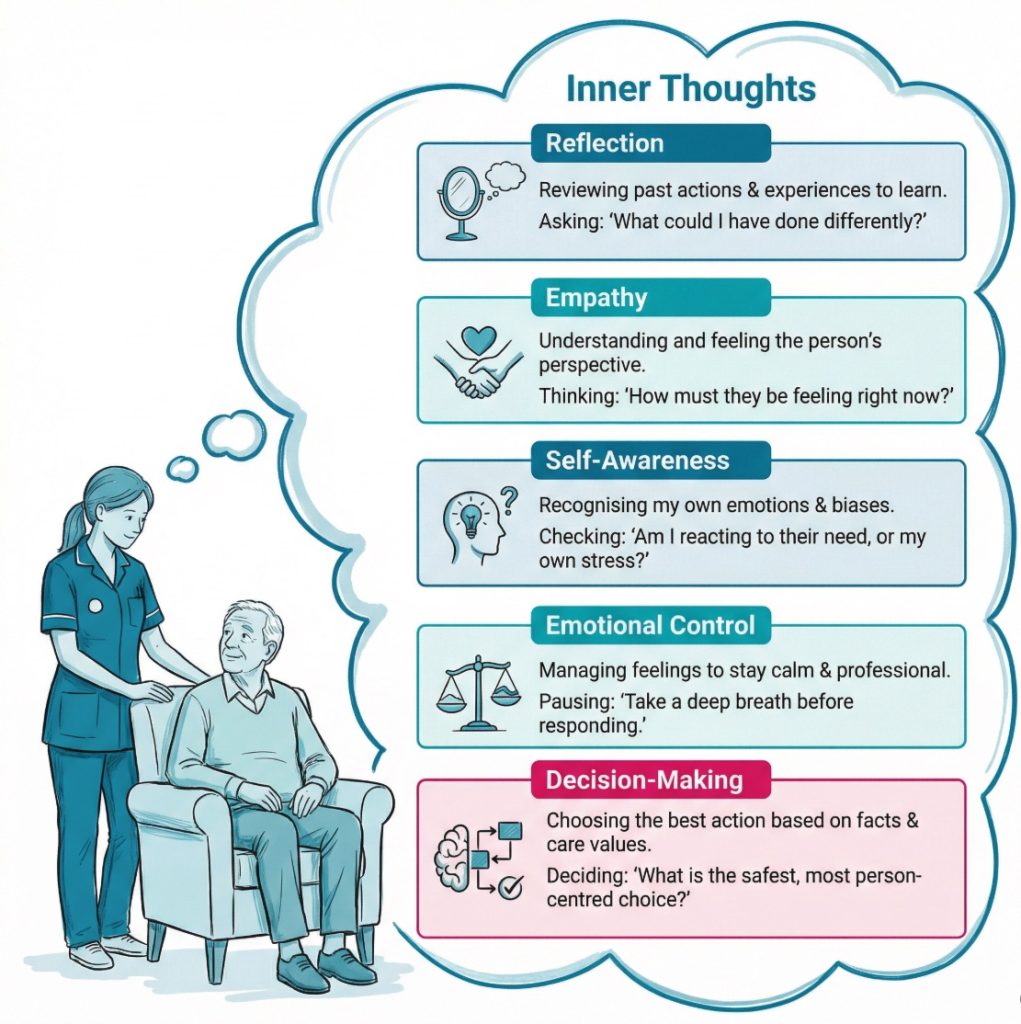
What intrapersonal communication looks like in care work
In care settings, intrapersonal communication shows up in small, ordinary moments. A nurse may think, “Keep this simple. They already look overwhelmed.” A support worker may notice irritation rising and think, “Pause. Don’t answer sharply.” A practitioner may leave a meeting and ask themselves, “Did I really listen, or did I jump to a conclusion?”
This inner dialogue can happen before, during and after an interaction. Beforehand, it helps staff prepare. They may think about the person’s needs, likely worries or preferred way of communicating. During the interaction, it helps them monitor their own emotional state. Afterwards, it supports reflection on what went well and what needs to change.
“Good care often starts with a pause that nobody else sees.”
This is closely linked to emotional awareness. Staff who notice their own reactions are usually better placed to respond with care rather than impulse. Meanwhile, a person receiving support may be dealing with fear, shame or confusion that never gets said aloud. The NHS page on communication difficulties shows why spoken words are only one part of good communication.
It also connects to person centred care. Workers often support people whose routines, beliefs and communication styles differ from their own. Private reflection can help stop personal preferences from taking over. A worker may think, “This is not how I would choose it, but my role is to respect the person’s choices where possible.” That keeps the focus where it should be.
For the person receiving care, intrapersonal communication can shape confidence and coping. Someone who tells themselves, “I can ask for help”, may engage more fully. Someone who thinks, “They won’t listen”, may say very little. Staff may never hear those thoughts directly, yet consistent respectful care can influence them over time.
The table below shows how intrapersonal communication may appear in everyday care work.
| Situation | Inner response | Possible effect on care |
|---|---|---|
| A person becomes angry during personal care | “They may feel exposed or frightened” | The worker is more likely to slow down and preserve dignity |
| A family member challenges a decision | “Listen first before defending the plan” | The conversation may stay calmer and more productive |
| A staff member feels overwhelmed | “Focus on the next safe step” | The response is steadier and less reactive |
| A review meeting feels rushed | “Have I really heard what this person wants?” | The worker may return to the person’s own priorities |
Granted, private reflection is not always neat or calm. Care work is busy, emotional and sometimes exhausting. Yet the habit of noticing inner thoughts can make day to day communication safer and more humane.
How it can be used to improve care, support and relationships
Intrapersonal communication can be used as a practical tool. It helps staff regulate emotion, question assumptions and think more clearly before they speak. That can improve the quality of support and reduce avoidable conflict.
One clear use is emotional regulation. Care work can involve grief, aggression, confusion, safeguarding worries and heavy workloads. In those moments, inner speech can either increase pressure or reduce it. A thought such as, “I can’t deal with this”, usually makes stress worse. A steadier thought such as, “Pause. Focus on the immediate need”, is more likely to support a calm response.
Another use is checking assumptions. People often form quick impressions. A worker may assume a person is rude when they are actually in pain. They may see a family member as controlling when that person is frightened and trying to protect someone they love. Private reflection creates a small gap between the first impression and the response. Sometimes that gap changes everything.
“A brief mental pause can prevent a poor response from becoming a poor experience.”
Reflective practice also grows from this inner process. Staff often think back over a difficult conversation and ask what shaped it. They may reflect alone, in supervision or with colleagues. The Skills for Care guidance on effective communication supports this wider point. Reflection helps staff learn from real situations rather than repeat the same pattern.
It can also help with professional boundaries. Some workers feel pressure to fix every problem or take distress personally. A more balanced inner response can protect both staff wellbeing and the person receiving support. A caveat here is that reflection alone is not enough. Training, supervision and team support still play a large part.
Ways intrapersonal communication may be used in care include:
- Preparing for difficult conversations: Staff may mentally rehearse clear, respectful wording before speaking about sensitive care needs. This can reduce anxiety and support a calmer discussion.
- Managing personal bias: Workers may notice an instant judgement and question it before acting on it. This can lead to fairer and more respectful care.
- Supporting de escalation: Quiet self talk such as “Stay calm” or “Listen first” can help lower tension. The person may then feel less threatened and more heard.
- Learning from experience: After a difficult shift or incident, reflection can help staff spot patterns. That can improve future communication and decision making.
A counter point is worth noting. Some people see this as overthinking and argue that good communication is simply about being kind and clear. There is truth in that. Kindness and clarity are central. Even so, inner dialogue often decides whether those qualities show up when pressure builds.
Benefits for people receiving care and for staff
When intrapersonal communication is used well, the effects build over time. People receiving care often experience better listening, more respect and steadier support. Staff may develop more confidence, better judgement and greater emotional resilience.
For the person receiving care, dignity is one of the clearest benefits. Staff who reflect before speaking are more likely to choose words that protect self respect. This is especially important during personal care, intimate support, end of life care and any situation where a person feels exposed or dependent.
Trust also grows through these small moments. People often notice impatience, facial expression and emotional tension even when very little is said. A worker who uses inner reflection to stay calm and attentive is more likely to create a sense of safety. The NICE recommendations on patient experience are helpful here because they focus on communication that fits the person in front of you.
For staff, intrapersonal communication can reduce reactive practice. Reactive practice happens when someone responds from stress, frustration or habit rather than judgement. On second thought, ‘reduce’ is the better word here than ‘prevent’. Pressure never disappears completely in care work. What changes is the worker’s ability to notice it and respond more carefully.
It can also support wellbeing. Persistent self criticism can wear staff down, especially in demanding services. Thoughts such as “I’m failing everyone” or “I should cope better” can build quietly over time. A more balanced inner voice can help staff recognise limits, seek support and process difficult days more safely. Related ideas appear in the Health and Safety Executive guidance on work related stress.
Benefits often include:
- Better empathy: Reflective inner dialogue can help staff see the person behind the behaviour. This often reduces conflict and improves relationships.
- Clearer decisions: Staff who pause to think through options may make more balanced choices. This is useful when a situation feels tense or uncertain.
- Improved confidence: Regular reflection can help workers notice strengths as well as gaps. That tends to build steadier professional confidence.
- More consistent support: Staff who know their own triggers are less likely to give mixed responses. Consistency can help people feel secure and understood.
- Stronger involvement for the person: When staff communicate with care and clarity, people may feel more able to ask questions and take part in decisions. The NICE shared decision making guidance links closely with this idea.
“People are more likely to speak up when care feels calm, respectful and predictable.”
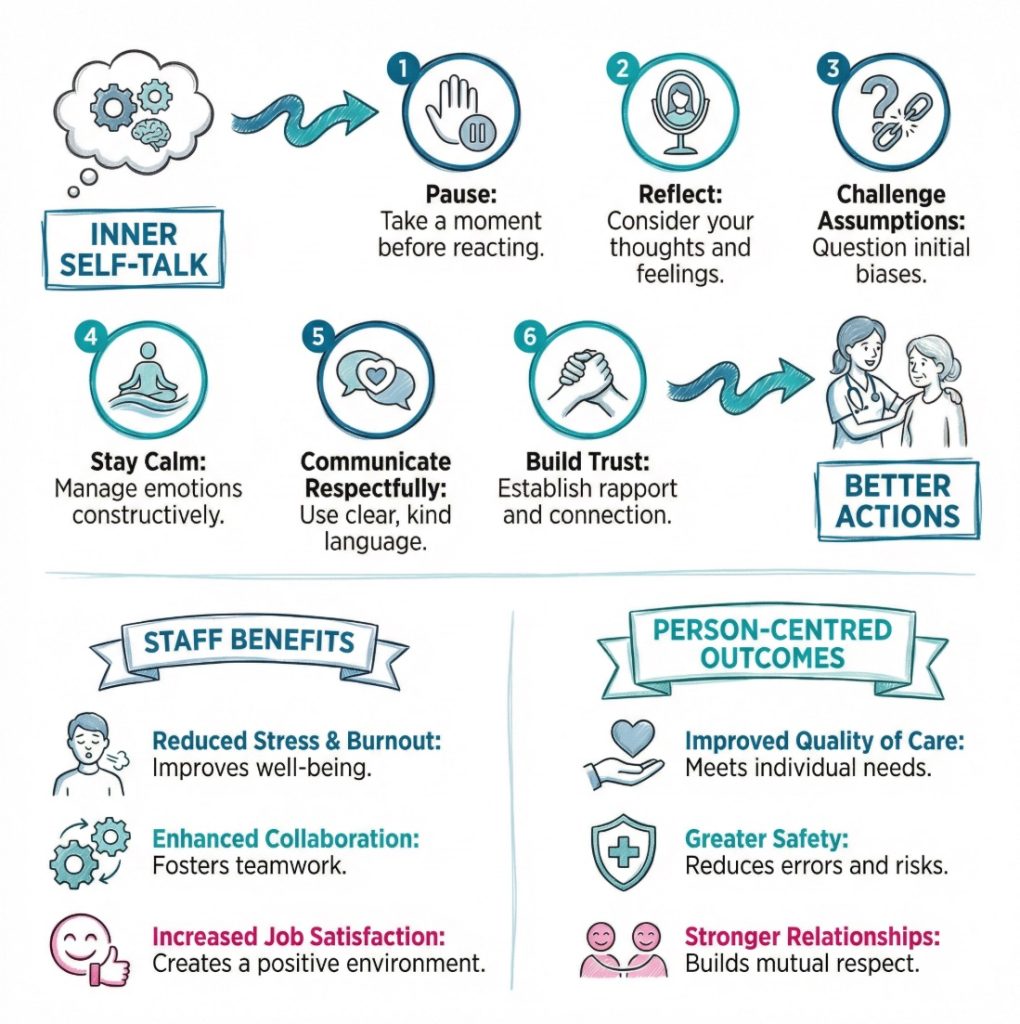
Challenges and limits in care settings
Intrapersonal communication can be helpful, but it is not always positive. Inner thoughts can be harsh, biased or based on incomplete information. In a busy care setting, those private messages can shape behaviour before anyone notices what is happening.
Negative self talk is one challenge. A worker under pressure may think, “I always get this wrong” or “There is no point trying.” Those thoughts can narrow attention and reduce patience. The person receiving care may then experience the worker as detached or abrupt, even when that was not the worker’s intention.
Unconscious bias is another issue. People can make fast judgments about age, disability, mental health, language, appearance or lifestyle without fully realising it. Private reflection can help challenge those assumptions, but it can also reinforce them if it goes unchecked. The Skills for Care person centred resources are relevant because they keep the person, rather than the worker’s assumptions, at the centre.
Stress narrows thinking too. When staff move quickly from one task to the next, reflective thought can become short and defensive. The inner message may shift from “What does this person need?” to “How do I get through the next ten minutes?” That response is understandable. Still, it can reduce care quality if it becomes the norm.
There are limits to what private reflection can do on its own. A member of staff may think carefully and still need training, supervision or clearer systems. A person receiving care may have negative self talk linked to trauma, illness or long term disadvantage. Respectful communication may help, but it may not remove deeper distress. So intrapersonal communication should be seen as one part of good care rather than the whole answer.
Common mistakes include:
- Overthinking: Too much self questioning can make staff hesitant. That may delay a response or reduce confidence.
- Personalising behaviour: Staff may take anger or distress personally instead of seeing the wider context. This can damage the relationship.
- Ignoring emotional impact: Some workers focus only on tasks and avoid reflection altogether. Over time, this can reduce empathy and increase exhaustion.
- Sticking with first impressions: An early judgement can harden into a fixed view. That can affect fairness and the quality of support.
- Using harsh self talk: Persistent self criticism can affect mood, concentration and communication. The Mind guidance on improving self esteem gives useful background on how inner beliefs shape wellbeing.
How to strengthen intrapersonal communication in everyday work
Stronger intrapersonal communication usually develops through habit. It grows when staff notice their thoughts, test them and choose a better response. Nothing dramatic. Just repeated small changes.
A good starting point is self awareness. Staff can begin by noticing what usually happens in stressful moments. Do they become defensive, rushed, self critical or avoidant? Do they assume they already know what the person means? Once those patterns are visible, they are easier to challenge.
Reflection after events also helps. This can happen informally after a conversation or more formally in supervision, a debrief or written reflection. The aim is not to judge yourself harshly. It is to understand what happened and how your private responses shaped the interaction. The NHS England summary on spoken communication and patient safety supports the wider link between communication, safety and empathy.
Supportive workplaces make this easier. When teams treat reflection as normal, staff are more likely to talk honestly about pressure, uncertainty and emotional strain. Training on communication, equality, trauma informed care and emotional wellbeing can also improve the quality of private reflection because staff have better ways to interpret what they notice.
For people receiving care, staff can support healthier inner dialogue indirectly. Clear explanations, respectful language, reassurance and involvement in choices may help a person feel more capable and less afraid. Over time, someone who once thought, “My views won’t count”, may begin to think differently.
A simple checklist can help staff reflect after a difficult interaction:
- Notice the first reaction: What did you feel straight away? This can reveal stress, fear or frustration before it shapes behaviour.
- Check the assumption: Was your first interpretation the only possible one? Another explanation may fit the situation better.
- Recall the person’s perspective: How might the interaction have felt from their side? This keeps the focus on the person, not only the task.
- Review your response: What did you say or do next? This helps link private thoughts to visible behaviour.
- Pick one change: What would you repeat or do differently next time? Small changes are often easier to sustain.
Practical takeaways include:
- Pausing before responding: A short pause creates space to think rather than react. That often leads to calmer communication.
- Using balanced self talk: Realistic inner messages can steady emotions. They do not remove stress, but they can stop stress from taking over.
- Reflecting regularly: Reflection helps staff learn from everyday situations. This can improve both confidence and quality of care.
- Seeking feedback: Colleagues or supervisors may notice patterns that the individual misses. Honest discussion can deepen self awareness.
Conclusion and next step
Intrapersonal communication is the private mental conversation that shapes how people see themselves, other people and the situations they face. In health and social care, it influences empathy, emotional control, judgement and the quality of relationships. It affects the worker’s behaviour and it can affect how safe, heard and respected the person receiving care feels.
Used well, it helps staff pause, think clearly and respond with more sensitivity. Used badly, it can feed stress, bias and misunderstanding. That is why it deserves close attention within communication training, reflective practice and day to day supervision.
The strongest next step is usually a simple one. Notice the private thoughts that appear before, during and after difficult interactions. Then look at how those thoughts shaped the response. Small changes in that inner conversation can lead to more respectful care, steadier relationships and better support for both staff and the people they serve.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.
Free Communication Skills Training Course
Start a free course with Care Learning today. Certified training with interactive elements, videos and mobile friendly.






