
Institutional discrimination in health and social care is unfair treatment that grows out of an organisation’s rules, routines, culture or systems, so that some people are placed at a disadvantage again and again.
This is wider than one worker being rude, biased or openly prejudiced. It describes a service that, often without saying so, works more smoothly for some groups than for others. The unfairness may sit in referral systems, assessment tools, appointment methods, care planning, complaint handling, communication, staffing patterns or everyday routines.
Health and social care settings bring this issue into sharp focus. People often rely on services when they are ill, distressed, in pain or unable to manage without help. If the service is set up in a way that overlooks their needs, the result can be poor care, confusion, delay, humiliation or avoidable harm.
Institutional discrimination can affect people because of race, disability, age, sex, religion or belief, sexual orientation, gender reassignment, pregnancy and maternity, or other protected characteristics under the Equality Act 2010. The Act covers discrimination in services and public functions, not only in employment. The Human Rights Act 1998 is relevant too, because health and social care can affect dignity, privacy, family life and personal autonomy.
There is a simple way to separate this from personal discrimination. Personal discrimination is about what one person says or does. Institutional discrimination is about what the system keeps producing. A worker may be polite and well meaning, yet the service may still leave some people less heard, less informed or less safe.
A service may claim that it treats everyone the same. That sounds fair at first. On second thought, it can hide a problem. People do not all arrive with the same needs, the same communication style, the same level of confidence or the same access to support. Equal care often means different support, not identical treatment. That is where this topic starts.
Why does institutional discrimination happen in care services?
Institutional discrimination rarely appears overnight. It usually grows through habits, routines and assumptions that no one has stopped to question. Staff may inherit working methods that seem normal because they have been used for years. Managers may look at whether a policy exists and stop there. Meanwhile, people using the service may keep having the same poor experiences.
One cause is the way services are often built around a “typical” service user. That model may suit people who can hear clearly, read standard letters, speak English confidently, use a phone, attend at short notice and explain their needs quickly. Many people cannot do all of that. A Deaf person may need a British Sign Language interpreter. A person with dementia may need repetition and time. A person with autism may need clear preparation and a calmer environment. A person with a learning disability may need easy read information.
Another cause is pressure. Short staffing, high demand and task based routines can push workers towards shortcuts. They may rely on labels such as “difficult”, “non compliant” or “frequent caller” instead of asking what is making the situation hard. Those labels can spread through records and handovers. Once that happens, the system starts to shape how the person is seen.
Culture plays a large part as well. If staff hear phrases such as “we treat everyone the same here” or “that family always complains”, the tone of the organisation can shift. Some concerns are then brushed aside before they are explored properly. Granted, consistency has value. Services need reliable systems. Yet a rigid system can become unfair when it leaves no room for different needs.
Leadership can either expose the problem or let it settle. A service may have equality policies, complaints procedures and training records. That still does not prove that people receive fair care. The real test is what happens on the ward, in the clinic, in the care home, during a home visit or at the point of discharge.
Some common reasons include:
- Standard systems with little flexibility: A pathway may suit people with straightforward needs but fail those who need extra support with communication, mobility or decision making.
- Poor workforce knowledge: Staff may know the language of equality but not recognise how discrimination shows up in records, routines and decisions.
- Weak challenge culture: Workers may notice unfair patterns but stay silent because they do not feel supported to raise concerns.
- Poor use of data: An organisation may not review waiting times, complaints, safeguarding concerns or outcomes by group, so repeating inequalities stay hidden.
- Task first practice: Staff may focus on finishing visits or completing forms and lose sight of the person in front of them.
Bit by bit, these features shape the service. Then the pattern becomes hard to ignore.
What does institutional discrimination look like in health and social care?
Institutional discrimination can appear almost anywhere in a care journey. It may affect access to the service, the first assessment, the way information is given, the language used in records, the design of care plans, the handling of complaints or the way safeguarding concerns are recognised. It often looks ordinary from inside the organisation. It feels very different to the person on the receiving end.
In a GP surgery or outpatient clinic, the problem may start with the booking system. A phone only route can exclude people with hearing loss, anxiety, language barriers or limited access to technology. A short appointment can leave little time for someone who needs support to explain symptoms. A letter in complex language may be unreadable for a person with low literacy, sight loss or a learning disability.
In hospital, the pattern may show through rushed communication, poor use of interpreters, visiting rules that overlook the person’s support network or discharge planning that assumes everyone can manage in the same way. In a care home, it may appear in meal options, personal care routines, fixed activity programmes or assumptions about religion, sexuality, culture and family life. In home care, it may show through short visits, frequent staff changes and care plans written for the service’s convenience rather than the person’s daily reality.
A frequent example is indirect discrimination. A rule may apply to everyone in exactly the same way and still disadvantage certain groups. A “one letter, one appointment, no exceptions” system sounds neutral. It can still work badly for people with memory problems, visual impairment, communication needs or unstable living arrangements.
Some realistic examples show how this can happen:
- Hospital setting: An older patient with hearing loss is given medication information quickly at the bedside. No one checks whether they have heard it properly. No adapted written information is offered. Staff record that the patient was informed, but the patient leaves without a clear idea of what to do.
- Care home setting: A resident is offered the same narrow menu every week. Their religious needs and lifelong food preferences are treated as awkward extras. Over time they eat less, feel sidelined and stop asking.
- Mental health setting: A person from a minority ethnic background says they feel frightened and misunderstood. Staff record them as “agitated” and “resistant” without exploring trauma, communication issues or previous bad experiences with services.
- Home care setting: A person with a learning disability has a care plan written in complex language. Different carers arrive each day and speak mainly to a relative. Support is provided, but the person has little real control over it.
- Community setting: A woman’s pain is repeatedly minimised. Staff assume she is exaggerating. The failure is not only in one conversation. It sits in a wider pattern of who gets believed and who does not.
This can also link to diagnostic overshadowing. That means staff assume new symptoms are part of a person’s existing condition or disability, instead of exploring other possible causes. The effect can be unsafe as well as unfair.
How does institutional discrimination affect people receiving care?
The impact is often immediate. People may feel ignored, judged, rushed or spoken over. Some describe a service that never quite sees them properly. Others feel that they have to fight for basic adjustments, repeat the same information or rely on relatives to get simple points taken seriously. Small incidents build up.
Poor communication can lead to poor care. A person who does not understand information about medication, treatment or support cannot make proper choices. A person who is not believed may face delays in assessment or treatment. A person whose behaviour is misunderstood may be labelled rather than supported. A person whose identity is overlooked may feel unsafe during intimate care or deeply uncomfortable in daily routines.
There is an emotional effect as well. Repeated unfair treatment can make people expect the worst from services. They may hold back important information, avoid appointments or turn up already anxious and defensive. Families and unpaid carers can lose trust too, especially if they feel every adjustment has to be argued for from scratch.
A fair counterpoint is worth noting here. Not every poor experience is evidence of institutional discrimination. Services do make mistakes, and some failures happen for reasons that affect everyone. Still, when the same kinds of people face the same barriers again and again, the pattern points beyond isolated error. That is where institutional discrimination becomes the stronger explanation.
The effect on daily life can be wide:
- Loss of dignity: People may feel reduced to a label, diagnosis or stereotype rather than treated as individuals.
- Reduced safety: Poor communication, delayed recognition of symptoms or missed adjustments can lead to avoidable harm.
- Less independence: People may be excluded from decisions because support has not been adapted to their needs.
- Emotional distress: Shame, fear, anger and exhaustion often follow repeated unfair treatment.
- Weaker trust in services: People may delay asking for help or stop engaging altogether.
This issue is not only about how care feels. It can shape outcomes, relationships and long term wellbeing.
What laws, standards and bodies are linked to this?
The most directly relevant law is the Equality Act 2010. It protects people from discrimination, harassment and victimisation on the basis of protected characteristics in services and public functions as well as employment. It also includes the public sector equality duty, which requires public bodies to think about how they can reduce discrimination and improve equality of opportunity.
The Human Rights Act 1998 is also tied closely to this topic. Health and social care can affect privacy, dignity, family life, autonomy and protection from degrading treatment. When people rely on others for intimate care, communication support or daily living, those rights move from theory into ordinary practice.
The Care Act 2014 is relevant in adult social care because it places wellbeing at the centre of local authority functions. That includes dignity, physical and mental health, protection from abuse and neglect, control over day to day life, family life and the suitability of living arrangements. Those themes sit very close to the discussion of institutional discrimination.
The Health and Social Care Act 2008 (Regulated Activities) Regulations 2014 are highly relevant too, especially the regulations on person centred care, dignity and respect, consent, safeguarding and good governance. CQC treats these as fundamental standards. They set the baseline below which care must never fall.
Several standards and bodies shape how this works in day to day care:
- Accessible Information Standard: This applies to NHS and publicly funded adult social care services and covers the need to identify, record, share and meet communication needs for disabled people and people with sensory loss.
- Reasonable adjustments: Services should take practical steps to remove barriers for disabled people rather than wait for problems to grow.
- Care Quality Commission: CQC regulates health and adult social care services and looks at areas such as dignity, equality, safety and quality.
- NHS England: NHS England publishes standards and guidance that affect access, communication and adjustment.
- Local authorities: Local authorities shape adult social care commissioning, assessment and support, so their systems can either reduce or reinforce inequality.
- Nursing and Midwifery Council: The NMC Code expects registrants to treat people fairly, listen to them and respect their needs and preferences.
- Health and Care Professions Council: HCPC standards require registrants to avoid discrimination and raise concerns when poor practice affects people.
These laws and standards do not remove discrimination on their own. They do, however, give a clear framework for what fair care should look like.
Useful further reading includes the Equality Act 2010 on legislation.gov.uk, the Human Rights Act 1998 on legislation.gov.uk, the Care Act 2014 wellbeing principle on legislation.gov.uk, the CQC guidance on regulations for providers and managers, the NHS England Accessible Information Standard, the SCIE guidance on tackling inequalities in care, the NMC Code and the HCPC standards of conduct, performance and ethics.
How might institutional discrimination play out in different settings?
The setting changes the details, but the pattern is often familiar. A service follows its usual routine. The routine suits some people. Others are left trying to fit themselves around it.
In hospitals, speed can hide unfairness. Staff may assume a patient has understood a treatment plan because they nodded. A relative who helps with communication may be treated as an optional visitor rather than part of safe care. Discharge planning may move ahead without checking whether the person can manage at home or has received information in a usable form.
In care homes, routine can become the problem. Set times for waking, bathing, eating and activities may fit the rota better than the resident. People whose faith, culture, gender identity, sexuality or communication needs fall outside the service’s usual habits may find themselves constantly adjusted around the home, rather than the home adapting around them.
In domiciliary care, time pressure is often central. A person with Parkinson’s, dementia or autism may need slower communication and familiar routines. A rushed visit from a different worker each day can turn ordinary support into something confusing or distressing. The care task is completed. The person is still not properly supported.
Mental health services can show the issue through assumptions about risk, credibility and behaviour. Fear may be recorded as aggression. Distress may be seen as refusal. Physical symptoms may be attributed too quickly to a mental health diagnosis. These patterns can change how people are treated from the first note in the record onwards.
Primary and community care often reveal barriers at the first point of contact. Phone first systems, digital forms and standard letters can exclude people before an assessment has even begun. After all, access is part of care.
A simple step by step example shows how the pattern can build:
- First contact: A person tries to access support but struggles with the service’s only booking method.
- No adjustment: Staff do not record or respond to the person’s communication or access needs.
- Rushed assessment: The conversation is brief, jargon heavy and shaped by assumptions.
- False reassurance: The person says “yes” or nods, and staff take this as full understanding.
- Poor planning: The care plan reflects the service routine rather than the person’s real needs.
- Breakdown later: Appointments are missed, support is poorly followed or risks increase.
- Blame shifts to the person: The record starts to describe them as difficult, unreliable or non compliant.
One missed step may look small. Put together, the pattern is hard to dismiss.
How could staff and organisations respond?
Staff may not control the whole system, but they are still part of how it works. The first task is noticing patterns rather than treating each incident as separate. If the same groups are being misunderstood, left waiting longer, denied adjustments or excluded from decisions, that should raise concern.
Staff also need to look carefully at language. Terms such as “challenging”, “frequent attender”, “attention seeking” or “non compliant” can shape the response of the whole team. Sometimes those terms reflect real difficulty. More often, they need a second look. They may say more about the service’s frustration than the person’s needs.
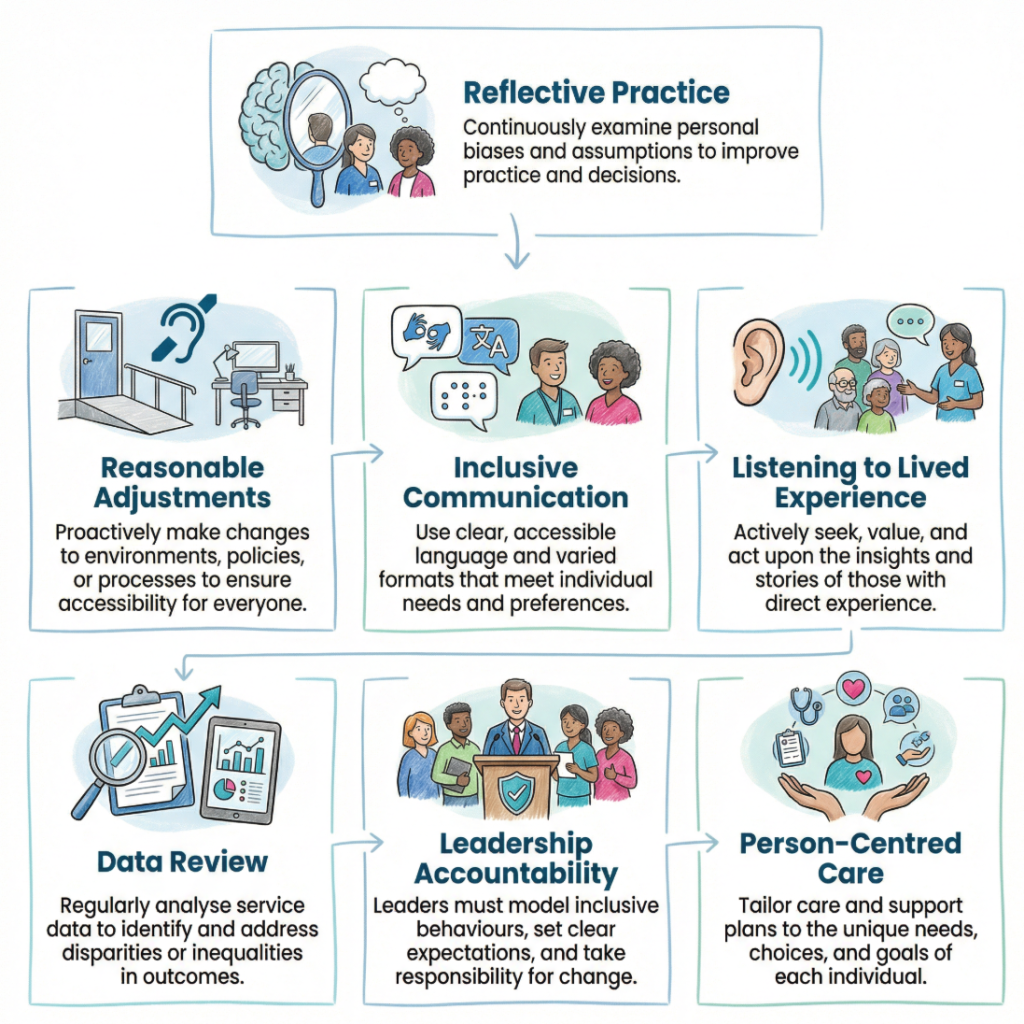
A useful response includes practical steps as well as reflection:
- Record needs clearly: Communication needs, reasonable adjustments, preferences and risks should be set out accurately and shared lawfully with relevant staff.
- Check understanding properly: A nod or short answer does not always show real understanding.
- Speak to the person directly: Relatives and carers may play a major part, but the individual should not disappear from the conversation.
- Raise concerns early: Supervision, incident reporting, safeguarding routes, complaints systems and whistleblowing procedures may all have a place.
- Review routines: If a rule keeps creating the same barrier, the rule needs attention rather than another apology.
- Use data honestly: Complaints, waiting times, safeguarding concerns, restraint, missed appointments and discharge outcomes can all show repeating inequality.
Organisations need to do more than publish policies. They need to test whether people actually experience care as fair and respectful. That means looking at lived experience, workforce culture, leadership behaviour and the quality of records, not just whether a policy folder is up to date.
A step by step approach may look like this:
- Spot the pattern: Ask whether the problem affects one person once or similar people repeatedly.
- Look at the system: Consider which rule, routine or assumption sits behind the difficulty.
- Check the person’s needs: Review communication needs, adjustments, protected characteristics and preferences.
- Write factual records: Keep notes clear, respectful and free from loaded labels.
- Raise the issue: Use the organisation’s reporting routes and supervision structures.
- Support fairness straight away: Put a practical adjustment in place where possible.
- Review what changed: Check whether the same barrier continues to affect the person or others.
Short, but important. A service becomes fairer when staff stop treating unequal outcomes as normal.
Where do services commonly go wrong?
A common mistake is confusing equality with identical treatment. A service may claim it is fair because everyone gets the same form, the same appointment length, the same leaflet or the same menu. Yet that approach can leave many people at a disadvantage from the start.
Another mistake is treating reasonable adjustments as optional extras. For disabled people, adjustments are often part of fair access. When communication or access needs are not identified, recorded and met, the service pushes the burden back onto the individual.
Services also go wrong when they rely too heavily on paperwork. Equality policies, staff training and posters on the wall can all look reassuring. They do not prove that people receive good care. The real test is whether the person feels heard, respected and included when they need help.
Some repeated errors are easy to spot once named:
- Ignoring repeated complaints: Similar complaints from the same group may be dismissed as isolated incidents instead of a pattern.
- Using stigmatising language: Terms such as “difficult” or “attention seeking” can harden poor attitudes and hide unmet need.
- Failing to review outcomes: Services may not compare access, delays, complaints or discharge experiences between different groups.
- Speaking over the person: Staff may talk mainly to relatives or other professionals and leave the individual out.
- Assuming cultural competence: Workers may believe they already understand a person’s background without asking what is actually important to them.
- Treating poor outcomes as inevitable: Some organisations come to expect that certain groups will engage less well or have worse outcomes. That expectation can become part of the problem.
Still, these mistakes are not random. They tend to grow where routines are rigid, pressure is high and challenge is weak. Naming them helps because it turns vague concern into something visible.
Final thoughts
Institutional discrimination goes to the centre of what good care is. Health and social care are not neutral systems. They affect people when they are often at their most exposed and dependent. If the service is unfair at that point, the damage can reach far beyond one appointment or one shift.
This topic also sharpens the meaning of person centred care. A service cannot claim to be person centred if it works well only for those who fit its default model. Fair care depends on recognising difference, adapting support and paying close attention to who is being left out.
For staff, this topic changes the questions worth asking. It is not enough to ask whether a task was completed. The better question is whether the care was fair, respectful and accessible to this person. That shift in thinking can alter records, conversations, decisions and outcomes.
For people receiving care, the effects are deeply personal. Institutional discrimination can shape safety, dignity, trust, choice and long term wellbeing. For organisations, it points to something equally concrete: the need to judge systems by what they produce, not by what they intend.
Care improves when patterns are noticed early, adjustments are treated as ordinary, and unequal outcomes are not waved away as bad luck. That is the centre of the issue. Clear enough. Human enough.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.






