
Policies in health and social care are written statements that set out how an organisation intends to work. They explain what staff are expected to do, what standards apply across the service, and why those standards are there. Put simply, a policy gives a clear line for practice. It should stop care from depending on guesswork, habit, or the personal views of whoever is on duty.
This has a direct effect on people who receive care. Many rely on staff for support with personal care, communication, medicines, safety, or daily routines. If there is no clear policy, one worker may respond well to a concern while another may miss it. One team may protect privacy carefully while another may treat it casually. That gap can unsettle people and raise risk. A sound policy helps close that gap.
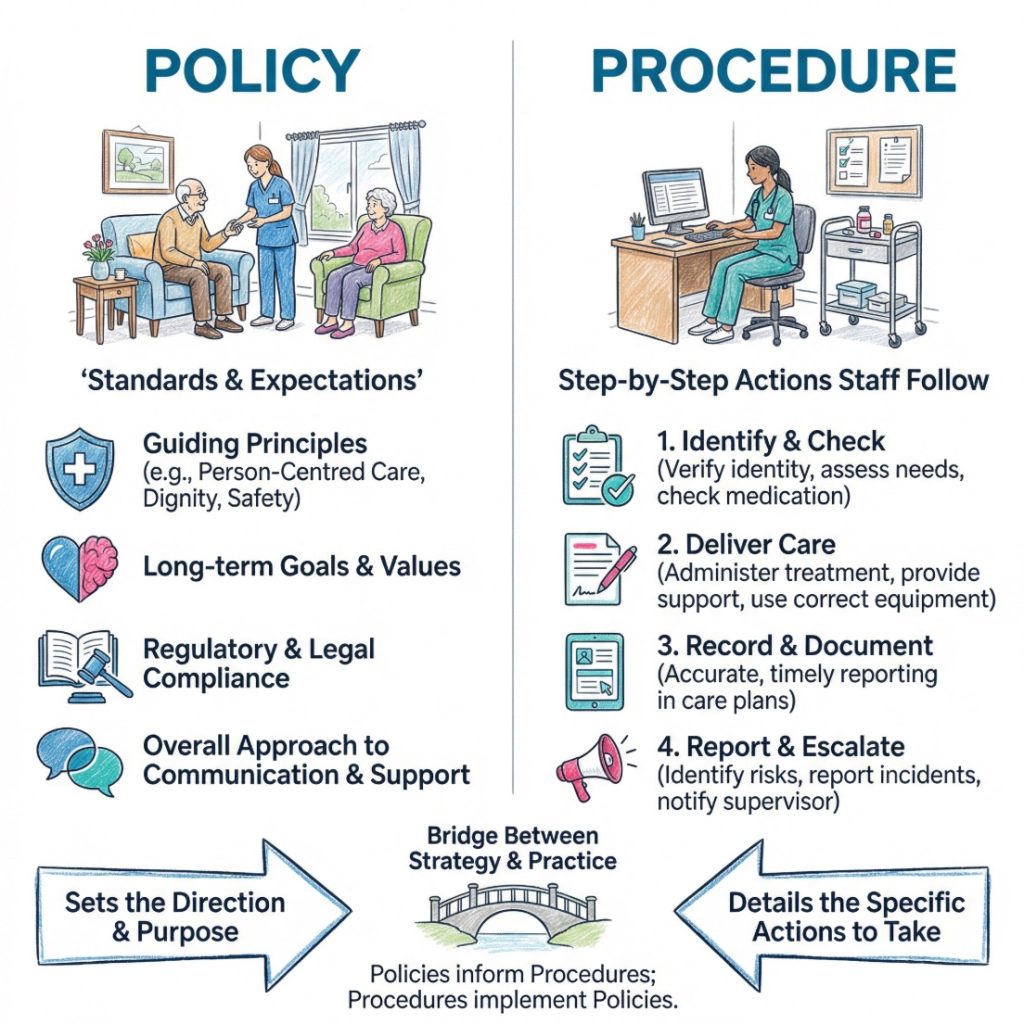
A policy is often discussed alongside a procedure, but the two are not the same. A policy sets the rule or position. A procedure sets out the steps that support it. For example, a safeguarding policy may state that every concern about abuse or neglect should be taken seriously and recorded properly. The linked procedure would usually cover who should be told, how the concern should be written up, and what should happen next. One sets direction. The other shows the route.
| Term | What it does | Example |
|---|---|---|
| Policy | Sets out the organisation’s standard, purpose, or position | A confidentiality policy says private information should be handled carefully and shared only when appropriate |
| Procedure | Explains the actions staff follow to meet that standard | A confidentiality procedure explains how records are stored, who can access them, and when information may be shared |
Policies also say a great deal about the culture of a service. A dignity policy points to the way privacy, respect, and choice should appear in daily care. A complaints policy shows whether concerns are welcomed and reviewed, or brushed aside. A medicines policy shapes how support is given and recorded. These are not decorative documents. They shape real behaviour in real settings.
“Policies turn values into daily routines.”
That is why services often connect policy work with wider standards and expectations, including the NHS Constitution for England, the Code of Conduct for support workers, and SCIE resources on safeguarding policy and procedures. Each source points to the same broad theme. Good care needs a clear framework, not loose custom.
Why policies are important for people receiving care and for staff
Policies help create consistency, and consistency can make a service feel safer. A person using a service should not receive warm, respectful support from one member of staff and careless treatment from another simply because expectations are vague. Policies aim to reduce that sort of uneven care. They give the whole organisation a shared standard, which can help people know what to expect.
The effect can be very practical. A moving and handling policy may reduce the risk of injury during transfers. An infection prevention policy may lower the chance of avoidable illness. A medication policy may support safer storage, administration, and record keeping. An equality policy may reduce discriminatory treatment and help staff respond properly to different cultural, communication, or religious needs. Each policy links back to the person’s daily experience of care.
For staff, policies provide structure. They can support new workers during induction, give experienced staff a reference point in difficult situations, and help managers review what should have happened after an incident or complaint. Still, a policy is not a substitute for judgement. Staff often need to think carefully about the person in front of them, the setting, and the level of risk. The document gives a foundation. It does not remove the need for thought.
A common criticism is that policies can become too bureaucratic. There is some truth in that. Some organisations produce long documents that are rarely read and barely linked to practice. Yet the answer is not to do without policies. It is to write them well, keep them clear, and use them in training, supervision, and review. On second thought, the real problem is rarely the existence of policies. It is poor policy design and weak follow through.
“Clear policies can steady practice when pressure rises.”
Some of the main reasons policies are used include:
- Safety: They set expectations around falls, medicines, infection, fire, safeguarding, and other risks so that staff have a safer basis for action.
- Consistency: They help different workers respond to similar situations in similar ways, which can make care more reliable for the person receiving it.
- Accountability: They make it easier to see what should have happened, which supports reflection, supervision, incident review, and learning.
- Respect for rights: They can support privacy, dignity, equality, choice, and involvement in decisions that affect daily care.
- Staff confidence: They can reduce uncertainty when staff face sensitive situations, complaints, or concerns about unsafe practice.
Further background can be found in the Skills for Care minimum standards, the NHS Constitution handbook, and SCIE guidance on safeguarding adults. Together, these sources show why policy work sits so close to quality, safety, and trust.
Common types of policies in health and social care
Most health and social care services have a wide set of policies because care work brings together risk, responsibility, communication, and personal support. Some policies focus on physical safety. Others cover information, behaviour, staffing, records, complaints, and equality. The list varies between settings, but the main themes stay fairly constant because the same core issues keep appearing in daily care.
Safeguarding policies are among the most significant. They help staff recognise signs of abuse, neglect, exploitation, or self neglect, and they set out how concerns should be handled. This has an obvious effect on the people receiving care. Missed signs can leave someone exposed to harm. It also shapes staff responsibility. Workers should know what concerns look like, how to record them accurately, and how to pass them on without delay. Linked policies often include whistleblowing, which supports staff who raise concerns about unsafe or poor care.
Confidentiality and information sharing policies are equally important. People often disclose highly personal details in care settings. Records may include medical information, family history, finances, behaviour, or intimate care needs. Policies in this area help services decide how information is stored, who can view it, and when it may be shared for safety reasons. Meanwhile, medicine management, infection prevention, and health and safety policies guide routine actions that can either protect people or expose them to avoidable harm.
Other policies shape the tone of the service. Equality, diversity, dignity, complaints, and person centred care policies influence how people are spoken to, how choices are respected, and whether concerns are heard properly. Granted, these can look less urgent than medicines or safeguarding at first glance. Yet poor communication or dismissive treatment can do real damage. Respect is not an extra.
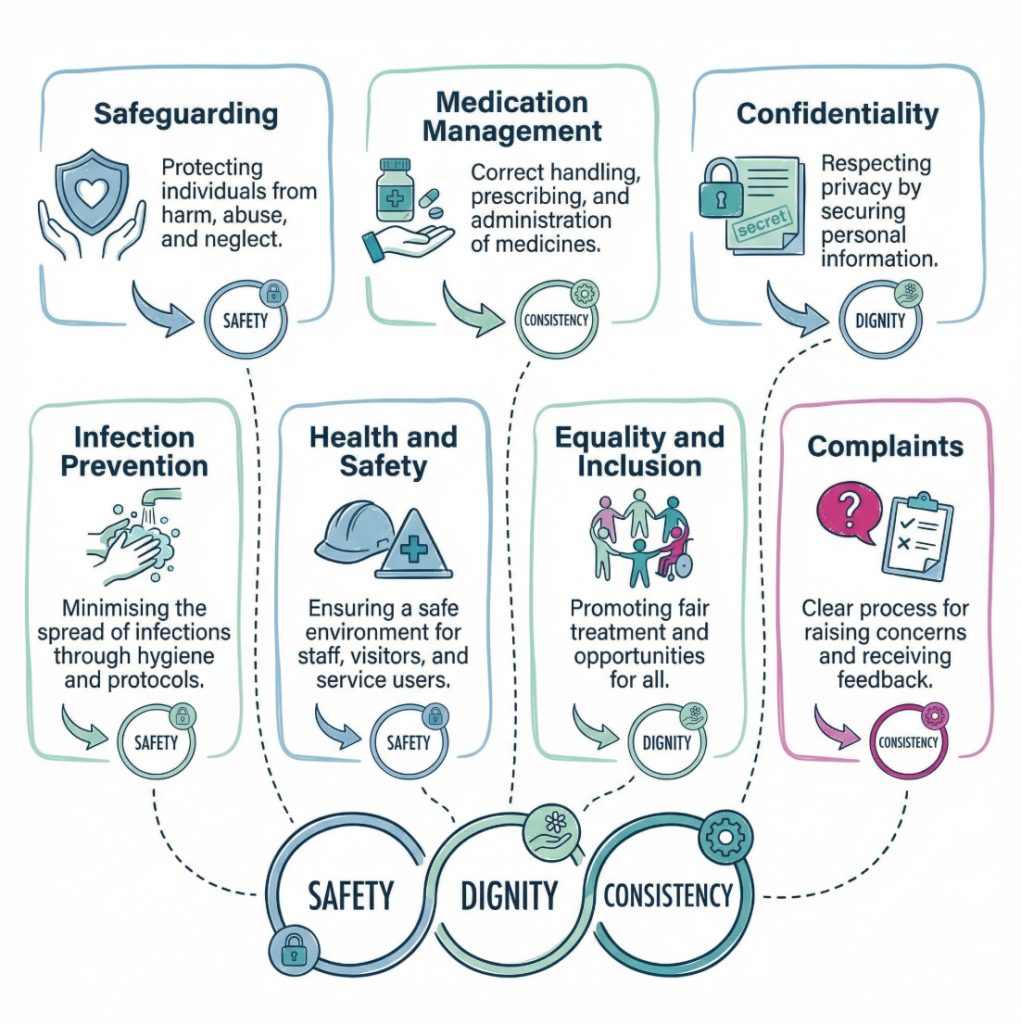
“People often judge a service by how well its policies show up in ordinary moments.”
Examples of common policy areas include:
- Safeguarding: Helps staff respond to abuse, neglect, exploitation, or self neglect and supports a safer environment for people at risk.
- Medication management: Covers storage, administration, recording, and error reporting so that medicine support is safer and easier to review.
- Confidentiality and data protection: Supports privacy and careful information sharing, which can strengthen trust between services, staff, individuals, and families.
- Infection prevention and control: Sets standards for hygiene, cleaning, protective equipment, and outbreak response to reduce the spread of illness.
- Health and safety: Covers accidents, equipment, risk assessment, fire safety, and environmental hazards that may affect staff and people using the service.
- Equality, diversity, and inclusion: Supports fair treatment and helps services respond better to different identities, beliefs, and communication needs.
- Complaints: Gives people and families a route for raising concerns and gives organisations a fair chance to review and improve practice.
Useful reading includes the NICE guideline on managing medicines for adults receiving social care, the NICE guidance on managing medicines in care homes, SCIE guidance on sharing information in safeguarding, and the Skills for Care safeguarding page. These links help show how policy areas connect to day to day care rather than sitting apart from it.
How policies are used in day to day practice
A policy only becomes useful when staff can apply it to real situations. Many organisations use policies during induction, supervision, training, incident review, and quality checks. This gives teams a shared point of reference. As a result, staff are less likely to rely only on memory, local habit, or verbal advice passed between colleagues. That can be especially helpful when events are sensitive, time is short, or views differ across a team.
Take a straightforward example. A worker notices unexplained bruising on a person who needs support with washing and dressing. A safeguarding policy should help the worker recognise that this is a concern, not a private suspicion to carry alone. The linked procedure should help with the next steps, including what to record, who to report it to, and what not to do. A complaints policy works in much the same way. If a relative is upset about missed care, staff can respond within a clear framework rather than reacting defensively.
Policies are also useful because services change. Risks change too. Staff teams shift, new equipment is introduced, care needs become more complex, and lessons emerge from incidents, feedback, and audits. Because of that, policies need regular review. A vague or outdated document can create a false sense of safety. Even so, review is only part of the picture. Staff also need to know where policies are kept, which ones relate to their role, and how those policies apply to the person in front of them.
A sensible step by step approach usually includes the following:
- Locate the relevant policy: Staff identify which document applies to the situation so that action is based on the correct standard.
- Read the practical section: Staff focus on the part that explains expectations, responsibilities, and any linked procedure.
- Record clearly: Staff write down what has happened in a factual way so there is an accurate account.
- Report through the right route: Staff pass the concern to the appropriate person or team rather than trying to manage it alone.
- Review and reflect: Managers and staff can look back at what happened and decide whether practice, training, or policy wording should change.
A brief example helps. In one care home, staff may have a falls policy that links risk assessment, observation, environment checks, and incident recording. If a resident falls at night, the policy gives the team a shared approach. It does not solve every decision, but it reduces confusion. Likewise, a confidentiality policy can help a support worker decide when a family member may be given information and when private details should remain restricted.
A useful checklist in this area often includes:
- Accessible documents: Policies should be easy to find, current, and written in plain language.
- Relevant training: Staff should be introduced to key policies early and revisit them during supervision or refresher training.
- Clear links to procedures: Staff need the practical steps as well as the principle behind them.
- Person centred use: Policies should support safe, respectful care for the individual rather than rigid, mechanical responses.
- Regular review: Organisations should revisit policies after incidents, complaints, audits, or changes in service delivery.
There are common mistakes too. Some services write policies that are too long to use. Others copy generic wording that does not fit the setting. Some fail to link policy to staff training. Not least, some treat policy review as a paperwork task rather than a way to improve care. Good policy work is quieter than that. It shows up in the small details of daily support.
Common mistakes when services rely on policies
Policies can support strong care, but only when they are current, clear, and used properly. One frequent mistake is treating a policy as proof of good practice. A service may have a folder full of documents and still deliver uneven care. Paper alone does not protect anyone. Staff need to know what the policy says, why it exists, and how it affects the person they support.
Another problem appears when organisations use inconsistent terminology or overload staff with repeated content. One document may refer to ‘service users’, another to ‘residents’, another to ‘patients’, and a fourth to ‘clients’. The language may sound minor, yet mixed terminology can make documents harder to follow. The same goes for repeated text copied between policies. It creates bulk without adding clarity. By contrast, cleaner wording makes it easier for staff to act confidently.
A few recurring weaknesses stand out:
- Outdated content: Old policy wording can leave staff following standards that no longer fit the service or current guidance.
- Poor access: A policy that is hard to find is rarely useful during a live incident or urgent concern.
- Generic wording: Broad statements without practical detail can leave staff unsure what to do next.
- Weak training links: Policies are less effective when induction and supervision do not refer back to them.
- Little review after incidents: Services miss learning opportunities when policies are not revisited after complaints, errors, or safeguarding concerns.
This is where a balanced view helps. Some people see policy work as heavy and repetitive. Others see it as the backbone of safe care. Both views contain part of the truth. Policy work can become repetitive when it is badly handled. Yet when the wording is clear and the training is solid, policies can help staff do difficult work more safely and more consistently.
Conclusion
Policies in health and social care set the standard for how an organisation aims to work. They shape the way staff protect people, respect privacy, manage risk, record concerns, and respond to complaints. They also give teams a shared framework, which can reduce confusion and support more consistent care across a service.
What gives policies their value is not the document on its own. It is the way the document is written, taught, reviewed, and used. Good policies help staff act with more confidence and help people receiving care feel safer, more respected, and better supported. Poor policies do the opposite. They add bulk without helping practice.
For readers looking at this topic, one useful next step is to compare a policy with its related procedure and notice how each one supports the other. That comparison often makes the whole subject clearer.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.




