
Duty of care in health and social care is the legal, professional and ethical responsibility to take reasonable steps to protect people from avoidable harm while giving care that is safe, respectful and suited to the person’s needs. It covers action and omission. It includes what staff do, what they fail to do, and how they respond when something is not right.
This sits at the centre of care because many people depend on staff for help with washing, eating, medicines, mobility, communication, decision making or protection from abuse and neglect. Kindness helps, yet kindness on its own is not enough. Safe care also needs observation, sound judgement, clear records, lawful consent, honest communication and timely reporting.
The topic appears early in workforce training for a reason. The Care Certificate standards include duty of care as Standard 3, and the CQC fundamental standards connect it to person centred care, dignity, consent, safety, safeguarding, governance and openness when things go wrong. These are not loose ideas. They describe what good care looks like from one shift to the next.
“Duty of care is not only about avoiding harm. It is also about noticing risk early, acting within your role and treating the person with dignity throughout.”
A simple way to frame it is this. If someone’s wellbeing may be affected by your work, there is a duty to act reasonably, follow safe systems and take concerns seriously. That applies in a care home, hospital ward, supported living service, GP practice, day service or a person’s own home. It also applies across roles, from care workers and nurses to social workers, therapists and registered managers. Professional standards from the NMC, the HCPC and Social Work England all reflect the same basic expectation of safe and accountable care.
Why duty of care is so important
Duty of care is important because poor care can cause harm very quickly, and the harm often starts with something small. A rushed handover. A missed fluid chart. A change in behaviour that nobody follows up. A worker using equipment without training. Each looks minor on its own. Together, they can place a person at real risk.
People receiving care may be ill, frail, disabled, distressed, confused or dependent on others for everyday tasks. Because of that, small omissions can have a big effect. The CQC guidance on safe care and treatment is built around this point. Providers are expected to assess risks, prevent avoidable harm, and make sure staff have the competence, skills and experience needed for safe care.
It also goes beyond physical safety. Care can fail a person without leaving a visible injury. A resident may be washed, dressed and medicated, yet still receive poor care if staff ignore privacy, speak over them, rush them or dismiss their distress. The CQC regulations page brings together the rules on person centred care, dignity, consent and safeguarding, which shows how closely these areas sit together.
For staff, duty of care gives a practical standard for everyday choices. It helps answer ordinary questions. Should this change be passed on now or later? Is this task within the worker’s competence? Does the person understand what is being proposed? Does this bruise need to be reported? Clear duties support better judgement, steadier teamwork and safer boundaries. The Code of Conduct for Healthcare Support Workers and Adult Social Care Workers sits in the same space. It links safe care to accountability, honesty and working within role limits.
“A duty of care shows itself in the small moments. The missed detail, the extra check, the concern that gets raised instead of ignored.”
What laws, standards and organisations shape duty of care
There is no single law called ‘the duty of care law’ that covers every detail of health and social care. Instead, duty of care is shaped by a group of laws, regulations and professional standards. In England, the Health and Social Care Act 2008 regulations are central for regulated services. These include Regulation 9 on person centred care, Regulation 10 on dignity and respect, Regulation 11 on consent, Regulation 12 on safe care and treatment, Regulation 13 on safeguarding, Regulation 17 on good governance and Regulation 20 on duty of candour.
The Care Act 2014 also plays a major part, especially in adult social care and safeguarding. It sets out the legal framework for care and support, including wellbeing, assessment and local safeguarding duties. Duty of care sits inside that wider structure because it is tied to assessment, care planning, prevention and safe support.
The Mental Capacity Act 2005 is another key part of the picture. It applies when there is doubt about a person’s capacity to make a specific decision. Staff are expected to support decision making where possible, avoid assuming incapacity and act in a person’s best interests if that person lacks capacity for the particular decision. The NHS guide to the Mental Capacity Act explains the broad principles clearly, including the point that an unwise decision does not by itself prove lack of capacity.
Professional bodies shape the subject too. The NMC Code is organised around prioritising people, practising effectively, preserving safety and promoting professionalism and trust. The HCPC standards of conduct, performance and ethics require practitioners to protect service users, communicate effectively, work within their knowledge and skills, delegate safely and report safety concerns. Social Work England’s professional standards set the threshold for safe and effective social work across roles and settings. Meanwhile, the Skills for Care duty of care workbook gives new staff a direct route into the topic.
How duty of care shows up in day to day work
Duty of care shows up in ordinary routines. A worker checks the care plan before starting. A nurse confirms identity before giving medicines. A support worker explains what they are about to do before helping with personal care. A domiciliary carer notices that a person is unusually drowsy and reports it. A social worker picks up signs that a family carer is overwhelmed and explores whether the current support is still safe.
These are not dramatic scenes. They are the daily fabric of safe care. The CQC page on safe care and treatment and the fundamental standards both point to the same pattern. Risks need to be assessed. Information needs to be shared. Staff need the right skills. People should not be exposed to avoidable harm.
Duty of care also includes the limits of the role. A care worker may spot a change in a wound, but that does not make the worker responsible for deciding clinical treatment. The duty lies in observing, recording and passing the concern on promptly. Equally, a support worker may be asked by a relative to alter a medicine dose or use specialist equipment without training. That request does not change the boundary of the role.
Some common examples make the point clearly:
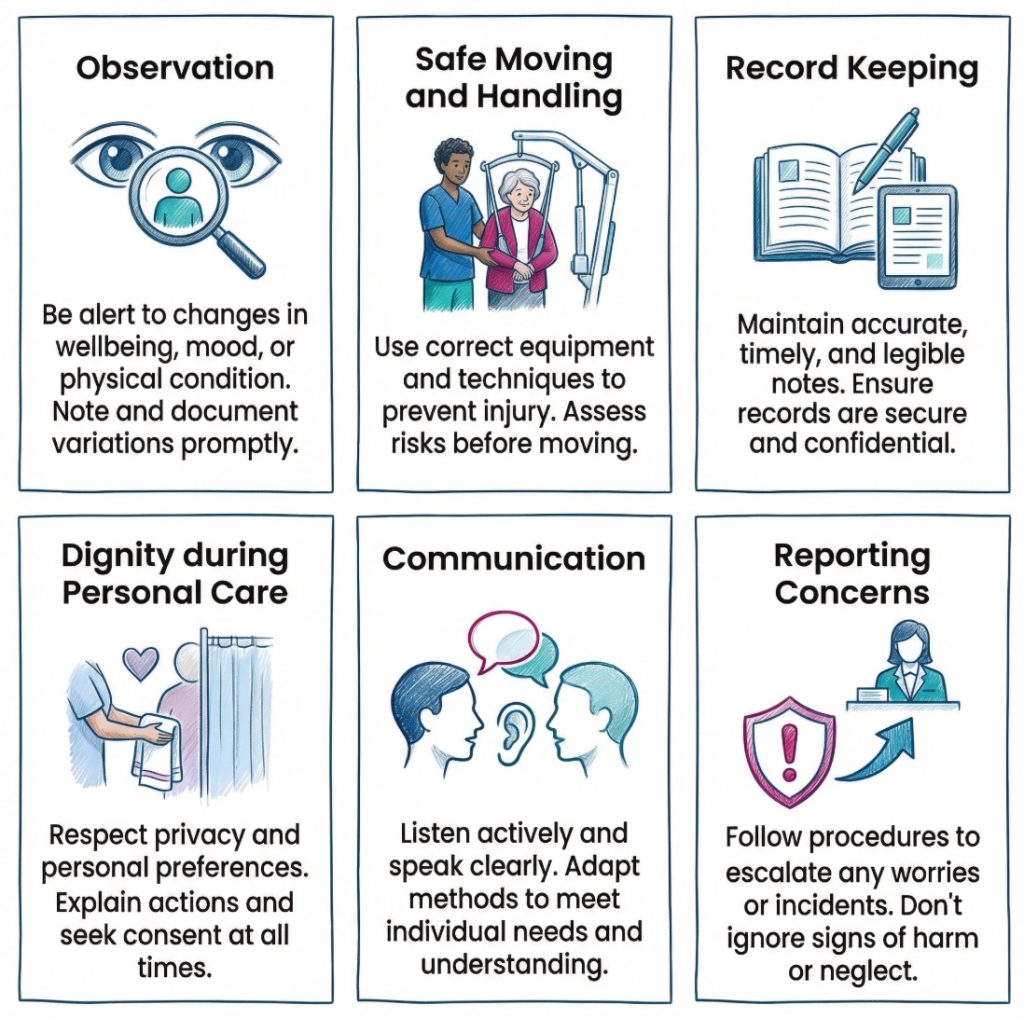
- Observing deterioration: A person who is usually alert becomes sleepy, confused and off their food. Duty of care includes noticing the change, recording it clearly and passing it on without delay.
- Protecting dignity: During personal care, staff knock first, explain what is happening and keep the person covered as much as possible. This protects privacy and reduces distress.
- Following care plans: Staff use the agreed moving and handling method rather than making it up as they go. This reduces the risk of injury for everyone involved.
- Sharing information safely: Relevant details are passed on during handover, but private information is not discussed where others can overhear.
- Respecting consent: Before care is given, staff check whether the person agrees and appears to understand what is being proposed.
- Raising concerns: If a colleague behaves roughly, ignores call bells or mocks a person, the duty includes reporting that behaviour through the right route.
“Good care is built from repeated ordinary acts. Clear notes, careful handling, privacy, consent and the confidence to speak up.”
More accurately, duty of care is a day to day standard, not a one off reaction to danger. It shapes the whole way care is given.
Where duty of care applies across settings
Duty of care applies across every health and social care setting, but the details can look different from place to place. In a care home, it may involve checking skin condition, preventing falls, monitoring food and fluid intake, supporting residents to keep routines, and making sure the environment is safe and respectful. The registered manager has an added layer of responsibility because systems, supervision and incident review sit within that role. CQC guidance on good governance links safe care to oversight, records, audit and learning.
In home care, workers often support people alone in their own homes. That changes the feel of the work. A domiciliary carer may arrive to find there is no heating, the medicines are unopened, or a relative is drunk and shouting. The worker may have no colleague beside them, yet the duty still stands. The response may involve keeping the person safe, recording facts and contacting the office or emergency services, depending on the risk.
Hospital settings bring another pattern. Observation, infection prevention, medication safety, communication between teams and response to deterioration are often central. A healthcare support worker who notices that a patient is clammy, disorientated and unsteady cannot brush that aside as tiredness. The duty is to alert a registered professional. Discharge planning raises similar issues. If mobility risk, carer strain or communication needs are missed, the care may fail after the person has left the ward.
Supported living and learning disability services often bring a different emphasis. Staff may support people to cook, travel, handle money or build daily living skills. Some people treat duty of care as a reason to remove all risk from these tasks. That sounds protective. Still, it can strip away independence and choice. The better approach is to reduce avoidable risk while keeping the person involved. The NICE guideline on shared decision making reflects the same principle in healthcare settings, where decisions should be made with people, not simply for them.
Social work adds another layer again. Assessment, safeguarding, care planning and work with families all sit close to duty of care. A social worker may need to balance respect for an adult’s choices with signs of coercion, neglect or self neglect. That requires clear records, lawful thinking and good professional judgement, not guesswork. Social Work England’s professional standards set out that safe and effective threshold across roles and settings.
When staff should act, report or escalate
Staff are expected to act when they become aware of a risk, a change in condition, unsafe practice or a situation where someone may not be safe. The concern does not have to be dramatic. It may be a pattern that has built up slowly, such as repeated dehydration, frequent rough handling, unexplained bruising or poor hygiene. First signs still count.
Timing makes a real difference. Waiting for proof can delay protection. The usual expectation is to observe carefully, record what has been seen or heard, and pass the concern to the right person without delay. If the risk is immediate, safety comes first. The CQC safeguarding pages and Regulation 12 both support that approach.
A simple sequence helps show how this works:
- Notice the concern: Pay attention to what has changed or what feels unsafe. This may be a physical sign, a missing medicine, a sharp change in mood or a pattern over time.
- Make the person safer: If there is immediate danger, take reasonable action within the role, such as calling for urgent help, staying with the person or removing a clear hazard.
- Record the facts: Write what was seen, heard or done. Keep the record accurate, clear and timed. Facts come first.
- Report to the right person: This may be the nurse in charge, line manager, safeguarding lead, on call manager or emergency service, depending on the setting.
- Escalate if needed: If the first response is poor or the concern is not taken seriously, the duty does not end there. Concerns may need to be taken further.
- Review and learn: Services are expected to look at what happened and whether training, staffing, care planning or communication needs to change.
A realistic example helps. A care worker sees that a resident’s heel is red and sore, and notices the person has not been repositioned as planned. The worker records the finding, informs the senior member of staff and checks that the concern has been acted on. If no one responds, escalation is still needed. Silence is not a neutral act here.
“Duty of care includes following a concern through. Passing on a message once is not always enough if the risk remains.”
How consent, capacity and choice fit into duty of care
Consent sits close to duty of care because safe care is not simply something done to a person. It should, where possible, involve their agreement and participation. Regulation 11 on consent and the CQC fundamental standards make that plain. Care or treatment should not be imposed as routine when the person can understand and decide.
This becomes more complex when a person refuses care or when there is doubt about mental capacity. Refusal does not automatically mean incapacity. The Mental Capacity Act 2005 and the NHS guide to the Act make clear that capacity is decision specific, people should be supported to make their own decisions where possible, and an unwise decision is not proof of incapacity.
This is where the subject can feel uncomfortable. Staff often want to keep people safe. By contrast, overprotection can remove independence, identity and control. A person may choose to walk with support rather than use a wheelchair all day. A man with dementia may refuse a wash at one point but accept it later with a familiar worker and gentler communication. A person in supported living may want to make tea, with support nearby, rather than have drinks made for them every time.
A short comparison helps here:
| Approach | What it looks like | Likely result |
|---|---|---|
| Safe, person centred support | Risk is reduced, the person is involved, and help is tailored to the situation | Safety is protected without wiping out choice |
| Overprotective support | Staff remove tasks or choices simply to avoid any risk | The person may lose confidence, skills and control |
| Careless support | Risks are ignored or poorly managed | Harm becomes more likely |
Some people argue that a strong duty of care pushes staff to stop people taking any risk at all. That reading is too narrow. Duty of care does not require blanket control. It requires reasonable action, lawful thinking and support that protects the person without wiping out choice. The NICE shared decision making guideline speaks to the healthcare side of that, while the Mental Capacity Act covers decisions for people who may lack capacity.
How duty of care links to safeguarding and candour
Safeguarding is one of the clearest expressions of duty of care. If abuse, neglect or improper treatment is suspected, the issue cannot simply be brushed aside or handled as gossip. Regulation 13 covers safeguarding service users from abuse and improper treatment, while the Care Act 2014 provides the wider legal framework for adult safeguarding in England.
Abuse can take different forms. Physical abuse, emotional abuse, sexual abuse, financial abuse, neglect, organisational abuse and self neglect can all appear in health and social care work. Signs are not always obvious. A worker may notice repeated bruising, fearfulness around one person, weight loss, poor hygiene, controlling behaviour from a relative, or sharp changes in mood and confidence. The duty lies in recognising the concern and using the reporting route set by the service.
Different roles pick up different signs. A care worker may spot rough handling. A nurse may notice pressure damage or poor pain control. A social worker may identify coercion or financial abuse. A registered manager may see patterns in incidents that point to a wider problem in the service. Each role sees part of the picture. Meanwhile, the person at risk may not feel able to say what is happening. That is one reason prompt action carries such weight.
Duty of candour is closely linked, but it is not the same thing. Candour is about openness and honesty when something has gone wrong. Regulation 20 on duty of candour expects providers and registered managers to act in an open and transparent way with people receiving care. In plain terms, that means explaining what happened, apologising where appropriate, giving truthful information and offering support.
“Safe care is not only about stopping harm. It is also about honesty afterwards, especially when trust has already been shaken.”
The link between the two is straightforward. Duty of care is about preventing harm and responding properly to risk. Duty of candour is about what should happen after harm, or potential harm, has occurred. A service that hides mistakes, blames individuals unfairly or keeps families in the dark is not meeting the standard of honest care that people should receive.
What commonly goes wrong
One common mistake is thinking duty of care only applies during emergencies. It does not. It applies during handovers, personal care, note writing, medication rounds, phone calls, discharge planning, home visits and safeguarding discussions. Omissions can be just as serious as obvious mistakes.
Another common mistake is confusing duty of care with doing everything for the person. Some staff become so focused on avoiding risk that they strip away everyday choice. That can look safe on the surface. Yet it may leave the person less independent, less confident and less involved in their own life. Duty of care does not require blanket control. It requires reasonable steps to reduce avoidable harm while respecting the person’s rights and preferences.
Working beyond competence is another frequent problem. Staff may feel pressure to ‘just get on with it’ during a busy shift. The HCPC standards are clear that practitioners should work within the limits of their knowledge and skills, and the NMC Code takes the same line on safety, delegation and professional accountability.
Other mistakes come up again and again:
- Poor recording: Notes are vague, late or missing key facts. This makes safe follow up harder.
- Weak escalation: A concern is mentioned once, informally, and then dropped when no one responds.
- Ignoring dignity: Personal care is treated like a task list rather than an interaction that affects self respect.
- Assuming consent: Staff carry out care because it is routine, without checking whether the person agrees or understands.
- Silence about colleagues: Poor practice is left unreported because staff do not want conflict.
- Loose confidentiality: Private information is shared in corridors, lifts or public spaces where others can hear.
A fair concern does come up here. Strong reporting duties can create fear if leadership is poor and staff expect blame rather than learning. Yet the answer is not less reporting. Instead, services need a fair culture where concerns are raised early, facts are checked properly and learning follows.
How learners can keep duty of care clear
A useful way to keep duty of care clear is to hold five plain questions in mind. What does this person need? What are the risks? What does the person want? What sits within this role? What needs to happen next? These questions bring the topic down from theory to ordinary care decisions.
The subject also becomes easier when it is seen as a thread running through other areas rather than a separate box on its own. It links closely to safeguarding, communication, confidentiality, consent, record keeping, risk assessment, professional boundaries and candour. The Care Certificate Standard 3 workbook takes that approach, and the 2025 Care Certificate standards place duty of care alongside person centred care, communication, safeguarding and privacy.
A short checklist can help fix the topic in place:
- Definition: Duty of care means taking reasonable steps to protect people from avoidable harm while giving safe and respectful care within the role.
- Why it exists: People receiving care may depend heavily on others, so staff actions and omissions can directly affect safety and wellbeing.
- What it includes: Observation, communication, consent, record keeping, risk awareness, safe boundaries and escalation of concerns.
- Where it applies: Care homes, hospitals, home care, supported living, social work and community services.
- What often goes wrong: Poor notes, weak follow up, unsafe delegation, ignored dignity, assumed consent and silence about poor practice.
- What supports it: The CQC regulations, the Care Act 2014, the Mental Capacity Act 2005, the Care Certificate and professional codes.
For many learners, the topic becomes clearer once it is tied to real situations. A missed pressure care check. A relative asking for information they should not receive. A patient who refuses treatment. A home visit where the person seems frightened but says little. Duty of care gives a route through each of these, not by offering a script, but by setting a standard for safe and accountable action.
Why duty of care stays central to good care
Duty of care stays central because it pulls together safety, dignity, consent, accountability and compassion in one working standard. It is not only about serious incidents. It shapes the ordinary quality of care people receive day by day, minute by minute.
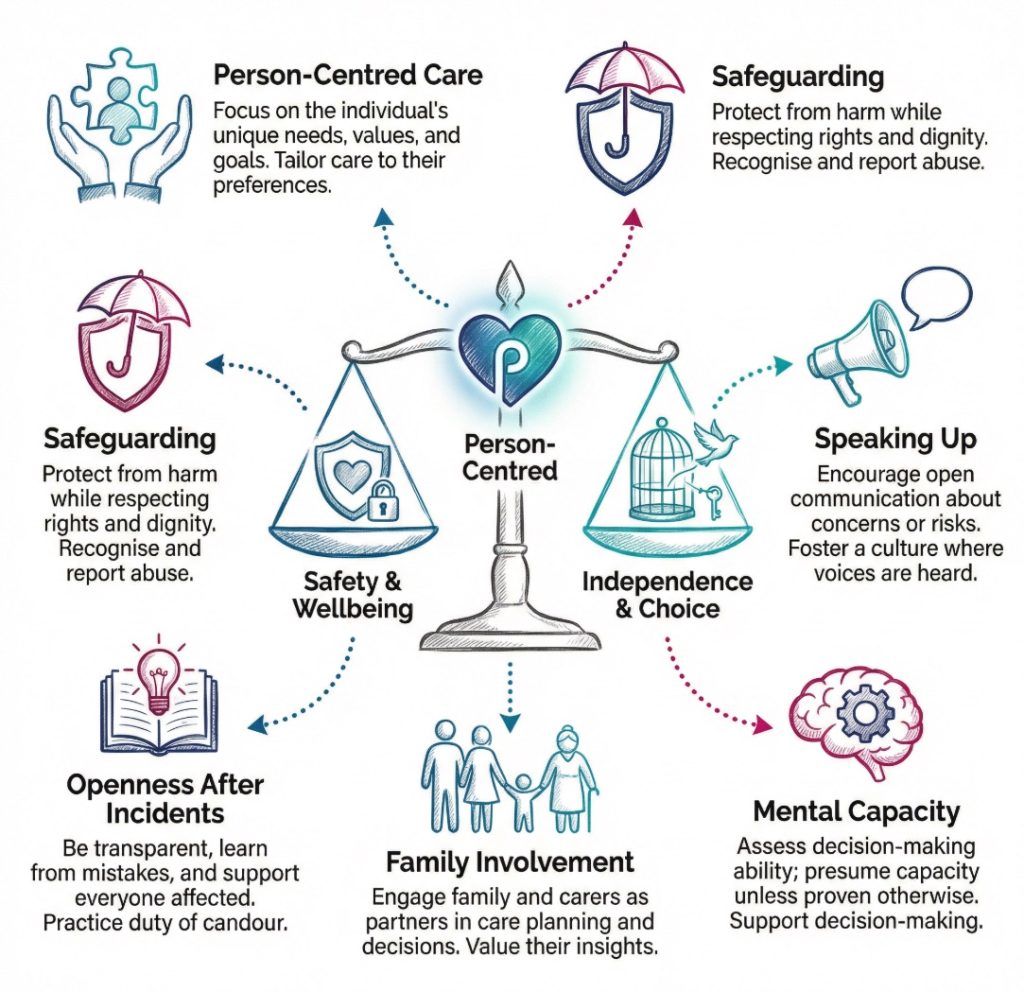
When staff notice changes, share information properly, respect privacy, follow care plans, work within competence and raise concerns, duty of care is being lived out in real work. When those things do not happen, harm can grow through action, omission or silence. The CQC fundamental standards and the Skills for Care materials on duty of care both point back to that basic truth.
The topic also helps connect law, standards and everyday care. It turns large ideas into concrete questions about what staff see, record, say and do. Rather than sitting as a dry theory in training, it becomes a way of reading real situations more clearly. That is why it remains one of the foundation subjects in health and social care, and why it keeps showing up across practice, supervision and regulation.
A sensible next step for anyone studying the topic is to link duty of care with safeguarding, record keeping, consent and the Mental Capacity Act. These topics share the same centre. People should receive care that is safe, lawful, respectful and honest. That is what duty of care asks for, every day.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.






