
Confidence has a direct effect on the quality of care people receive and the way staff carry out their role. It shapes how people speak, listen, make decisions and respond when something changes. In health and social care, people are often unwell, anxious, dependent on others, or unsure what will happen next. In that setting, confidence can change the whole experience.
Here, confidence is not about being forceful or acting as if you know everything. It is usually quieter than that. It means being steady, speaking clearly, asking sensible questions, and staying calm when a situation is difficult. It also applies to the person receiving care. When people feel confident, they are more likely to explain what they want, say when something feels wrong, and take part in choices about their care. Resources on person-centred approaches in health and care, shared decision making and accessible information all point towards the same idea. Care is safer and more respectful when people feel able to speak.
“Confidence helps turn care from a task into a relationship.”
A common counterpoint is that confidence can look risky if it tips into overconfidence. That is true. Poor care can follow when someone stops checking, stops listening, or assumes they are right. Still, proper confidence is different. It sits alongside competence, reflection and honesty. It gives people enough steadiness to act well without pretending they know more than they do.
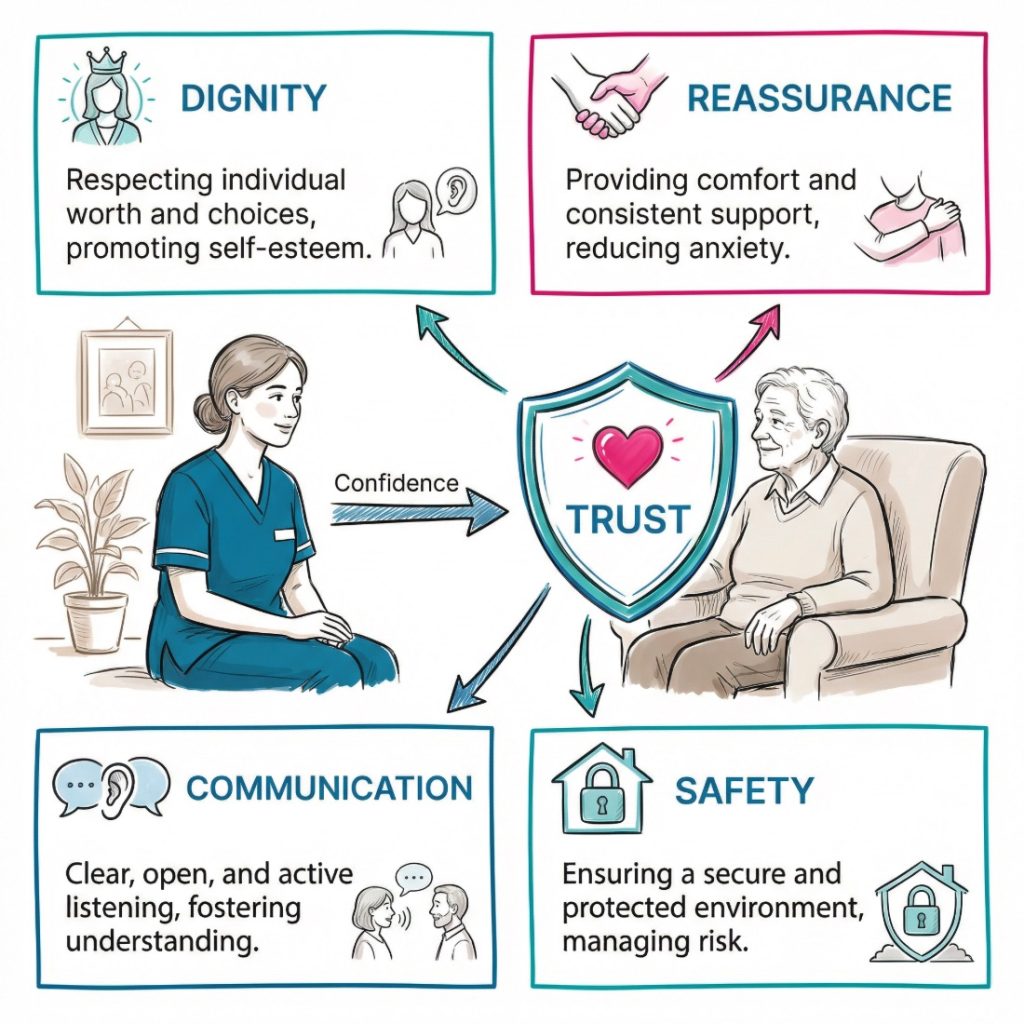
Confidence builds trust and a sense of safety
Trust often starts with small details. A calm greeting. A clear explanation. A steady tone. Time to listen. In health and social care, these details shape whether a person feels safe with the worker standing in front of them. If the worker seems unsure, distracted or rushed, the person may feel exposed, especially during personal care, support with mobility, medication, or emotional conversations.
Confident staff often make the experience feel more settled. They are more likely to introduce themselves properly, explain what is happening, check consent and respond in a way that reduces fear. That consistency helps people feel secure. For someone living with dementia, anxiety, a learning disability, trauma or a long term condition, that steady approach can ease distress and reduce confusion. Short, simple things. Yet they carry weight.
Trust also depends on whether the person receiving care feels safe enough to speak. A person-centred approach works best when the individual can say what suits them, what does not, and what they need changed. Guidance on involving people in their own care and person-centred care supports this view. When people feel included, care is more likely to reflect real needs rather than routine alone.
A small example shows this clearly. An older person may agree to a morning wash every day because they do not want to be difficult. A confident worker might notice hesitation, ask a simple follow up question and learn that the person has always preferred evenings. Nothing dramatic. But the result is more dignified care, less distress and a stronger relationship.
“People trust care more easily when they feel listened to, not managed.”
Useful signs of confidence in this area include:
- Clear introductions: Staff explain who they are and why they are there, which helps reduce anxiety and confusion.
- Steady communication: A calm tone and simple language can help people feel safe during difficult or personal tasks.
- Respect for consent: Confident workers are more likely to pause, check agreement and respond properly if the person hesitates.
- Support for personal choice: People are given space to say what suits them, which strengthens dignity and trust.
Confidence improves communication and advocacy
Communication sits at the centre of health and social care. Without it, needs get missed, risks go unreported and people can feel ignored. Confidence improves communication because it helps staff ask clear questions, listen properly and pass information on in a way others can use. It also helps people receiving care speak up about pain, fear, confusion, discomfort or concerns at home.
Some conversations are hard from the start. Pain, incontinence, safeguarding worries, memory loss, side effects, mental health and family conflict can all be difficult to raise. Staff who lack confidence may avoid these topics or ask about them too vaguely. People receiving care may do the same. That can leave serious needs hidden. Guidance on effective communication, the Care Certificate communication standard and shared decision making in the NHS all support the importance of clear, two way conversation.
Confidence also strengthens advocacy. Advocacy means keeping the person’s voice present in decisions about their care. That may involve noticing when consent has not been properly checked, speaking up when a person is being left out of a conversation, or making sure a quieter individual is not overshadowed by relatives or professionals. Staff need confidence to do that well. The person receiving care needs confidence too.
A caveat here is that confident communication should not become controlling communication. There is a difference between being clear and taking over. Strong care workers can explain options, ask good questions and leave room for the person to answer in their own way. That balance is often where dignity lives.
Mini case examples help show the difference:
- Pain reporting: A resident says they are “fine” during a medication round, but their face suggests otherwise. A confident worker notices the mismatch, asks again gently and records the response clearly.
- Family meetings: A daughter speaks for her father throughout a review. A confident practitioner brings the conversation back to him and checks his own wishes.
- Accessible information: A person with sensory loss receives information in a format they can actually use, which gives them a better chance to ask questions and stay involved.
“Confidence gives people the language and space to say what is really going on.”
Confidence supports person-centred care and independence
Good care is not only about completing tasks. It should fit the person’s routines, preferences, history and goals. Confidence supports this because it helps staff move beyond a checklist and have fuller conversations. Workers who feel secure in their role are usually more able to ask open questions, notice small preferences and adjust support without losing sight of safety.
That is especially important when care affects daily identity. Washing, dressing, eating, moving around, joining activities, speaking with family, using communication aids and choosing how the day runs are not minor details. They are part of how people keep hold of themselves. Resources on person-centred approaches and leading a person-centred service both reflect this wider view of care.
Confidence also protects independence. Staff sometimes step in too quickly because it feels faster, safer or more efficient. Yet doing everything for someone can reduce confidence over time. A person may stop trying, lose skills, or feel they no longer have any control. By contrast, confident staff are more likely to judge when to support and when to stand back. They can encourage a person to do what they can safely manage without making them feel tested or hurried.
On second thought, independence here is not always about doing every task alone. Sometimes it is about choice, pace and involvement rather than full physical ability. A person may need help dressing but still want to choose their clothes. They may need support with meals but still want to decide when to eat. Confidence helps staff notice the difference.
A short comparison shows how this plays out:
| Approach | What it can look like | Likely effect on the person |
|---|---|---|
| Low confidence support | Staff take over quickly and stick closely to routine | The person may feel passive, rushed or overlooked |
| Grounded confidence | Staff explain, encourage and adjust support around the person | The person is more likely to feel respected and involved |
Practical takeaways from this section include:
- Preserve routine where possible: Familiar habits can reduce distress and help people feel more secure.
- Support choice in small ways: Small decisions about clothing, timing or food can protect dignity and control.
- Avoid taking over too soon: Independence can shrink when staff step in before it is needed.
- Notice personal history: Knowing what people value can improve everyday care, not just care plans.
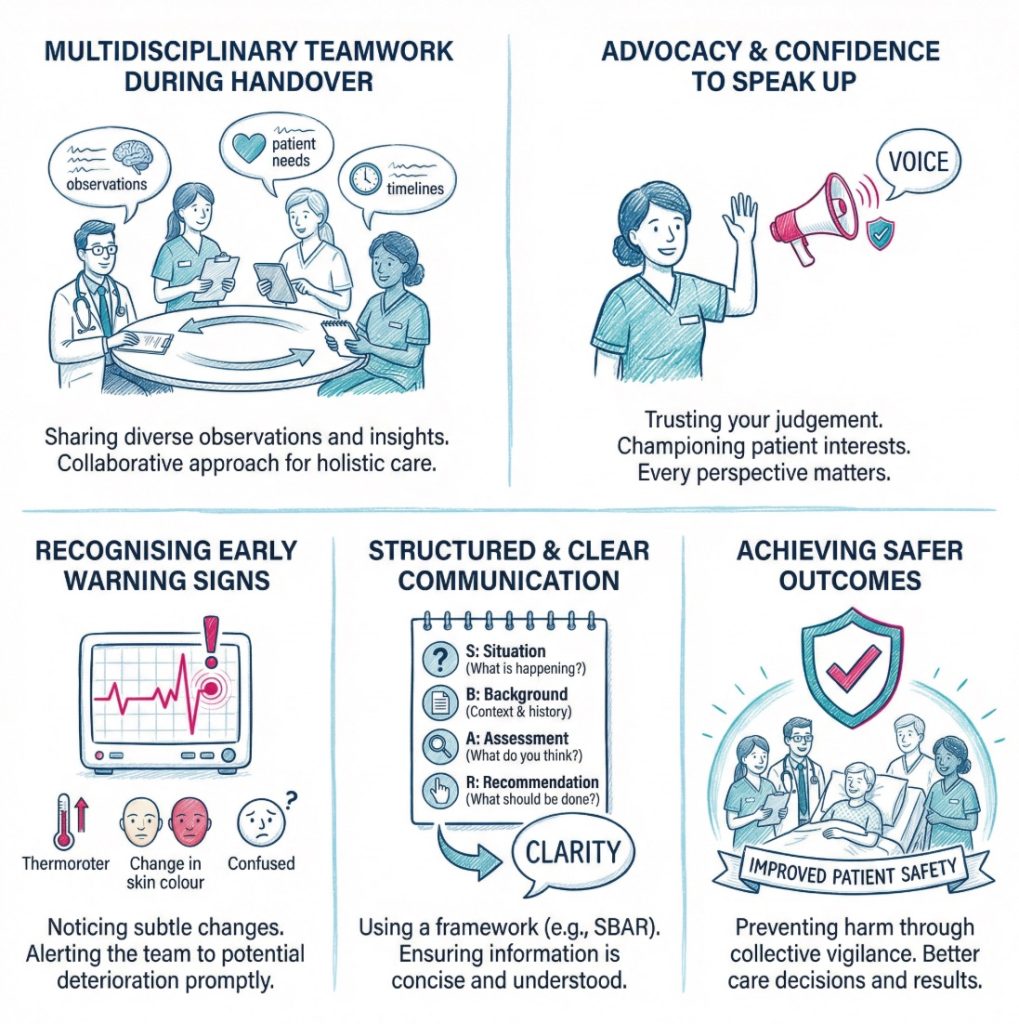
Confidence helps staff work together and speak up about risk
Health and social care depends on teams. One worker may spend the most time with a person, but safe care still relies on handovers, records, supervision and shared judgement. Confidence supports all of this. It helps staff say what they have seen, ask for help when they need it and raise concerns before a problem grows.
This is closely linked to safety culture. Pages on safety culture, improving patient safety culture and freedom to speak up all point to the same pattern. Teams work better when people feel psychologically safe enough to speak. If staff stay quiet because they fear criticism or feel unsure of themselves, warning signs can be missed. Often quietly.
Confidence in a team does not mean acting alone. It often means the opposite. A confident worker is more likely to say that a moving and handling plan is not being followed, that a medicine instruction looks unclear, or that a person seems less alert than usual. They are also more likely to say, “I’m not certain about this, can you check?” That sort of honesty protects people.
Meanwhile, the person receiving care benefits from better teamwork in ways they may never see directly. Handover becomes clearer. Concerns are followed up sooner. Records are more useful. Mixed messages are less common. The overall experience feels more joined up and less chaotic.
Warning signs of a low confidence team culture include:
- Silence after concerns are raised: Staff may stop repeating a concern if they expect to be ignored or criticised.
- Over-reliance on senior voices: Important details can be lost when only the most senior person speaks.
- Unclear handovers: Hesitant or vague updates can leave out details that other staff need.
- Fear of admitting uncertainty: People may stay quiet rather than ask for support, which can increase risk.
“A safer team is often a team where people can say, ‘I’m not sure’, without fear.”
Low confidence can affect outcomes for people and staff
Low confidence can change care in subtle ways. A worker may avoid difficult conversations, delay reporting a concern or rely too heavily on others to make decisions. They may stick rigidly to routine because they do not feel able to adapt. They may also struggle to challenge poor practice or explain care in a way that helps the person feel at ease. The task gets done, but the quality of the interaction drops.
For people receiving care, low confidence can lead to silence and withdrawal. Someone may say they are comfortable when they are not. They may avoid asking questions because they do not want to seem difficult. They may agree to plans they do not fully follow. Over time, that can weaken trust and reduce involvement in their own care. It can also affect dignity, because unspoken preferences are easily pushed aside.
The effect on staff can be serious too. Workers with low confidence may second guess themselves, feel more stress after routine tasks and become less willing to recover openly from mistakes. Granted, confidence alone does not solve heavy workloads or poor staffing. Those pressures are real. Yet confidence still shapes how people respond within those pressures. It can improve escalation, clearer records and safer teamwork even when the environment is demanding.
Common mistakes linked to low confidence include:
- Vague reporting: The worker senses a problem but describes it too loosely for others to act quickly.
- Avoiding advocacy: The person’s wishes are not brought forward when systems or routines take over.
- Task first care: Care is completed, but the person feels unseen because no one explores preferences properly.
- Doing too much for the person: Staff step in too early, which can reduce confidence and independence over time.
A short checklist can help frame what grounded confidence looks like:
- The person is included in conversations about their care.
- Questions are welcomed rather than brushed aside.
- Concerns are escalated when something changes.
- Support matches the person instead of the routine alone.
- Staff can admit uncertainty and ask for help when needed.
Confidence can grow through experience, support and reflection
Confidence is not fixed. It can be developed. In health and social care, it often grows through training, repetition, feedback, reflection and supportive leadership. New staff may begin with good intentions but little confidence in handling conflict, recording concerns, discussing risk or responding to distress. Over time, these skills can strengthen when people are properly supported.
Reflection plays a big part. It allows staff to look back at what happened, what worked, what felt difficult and what could be improved next time. This is not about over-analysing every shift. It is about turning experience into better judgement. Support from supervision, mentoring and team discussion can help with that. So can structured learning through resources such as the Care Certificate Standard 5 on person-centred care.
Confidence can also be built around the person receiving care. When information is clear, communication support is available and questions are treated with respect, people often become more able to take part in decisions. That is one reason accessible information and shared decision making are so relevant here. Confidence does not appear out of nowhere. People often gain it because the setting around them makes it easier to speak.
A practical step by step pattern can help explain how confidence develops:
- Learn the role: Knowledge reduces uncertainty and helps staff recognise what good care looks like.
- Practise with support: Repetition, feedback and supervision help turn knowledge into steady action.
- Reflect on experience: Looking back can sharpen judgement and improve future responses.
- Speak up earlier: Confidence often grows when concerns are raised and taken seriously.
- Keep the person involved: Care feels better and works better when the individual stays part of the conversation.
Conclusion and next step
Confidence is important in health and social care because it affects trust, communication, advocacy, independence, teamwork and safety all at once. It changes how staff present themselves, how clearly they communicate and how willing they are to raise concerns. It also changes how people receiving care experience support. When they feel secure enough to speak, ask questions and express preferences, care becomes more personal and more respectful.
The strongest form of confidence is not loud or rigid. It is calm, skilled and honest. It lets staff explain clearly, listen properly and admit when they need support. It gives people receiving care more room to keep their voice, their choices and their dignity. That is why confidence is woven through good care from start to finish.
A useful next step is to read the article again with one question in mind: where does confidence show up first, in communication, in teamwork, or in the person’s ability to speak for themselves? The answer is often all three.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.






