
The four stage mental health continuum describes mental health as a changing range rather than a fixed label. The four stages are healthy, reacting, injured, and ill. A person can move in either direction along that range over time.
This model is widely used because it gives a simple way to describe changes in mood, thinking, behaviour, sleep, energy, and day to day functioning. It does not diagnose a condition. It shows where a person may be at a given point and what their level of strain looks like.
Mental health rarely stays still. Stress at work, grief, physical illness, trauma, money worries, poor sleep, family pressure, or loneliness can all shift a person along the continuum. Support, rest, treatment, routine, safety, and connection can help move them back towards stability.
A moving picture of mental health.
The idea fits well with the broader approach taken by the NHS mental health pages, NICE guidance on mental wellbeing at work, and Skills for Care mental health resources. These sources describe mental health as part of everyday health, work, care, and relationships rather than a narrow clinical label.
“The continuum works because it shows change before crisis.”
Why the continuum gives a clearer picture of mental health
A simple well or unwell split misses too much. People often show early signs of strain long before they reach crisis point. They may still go to work, attend college, care for children, or keep appointments. Yet their sleep may be breaking down, their patience may be thinner, or their thinking may be less clear.
The continuum helps with that middle ground. It creates language for change that is concrete and easier to recognise. A person may move from healthy into reacting after a bereavement. Another may slip from reacting into injured after weeks of poor sleep and pressure. By contrast, someone living with a diagnosed mental health condition may still have long stretches in the healthy stage when symptoms are stable and support is in place.
This is one reason the model is useful in care services, workplaces, education, and family life. It supports better observation and better conversations. Instead of asking only whether a person has a mental illness, it helps people look at what has changed and how much impact that change is having.
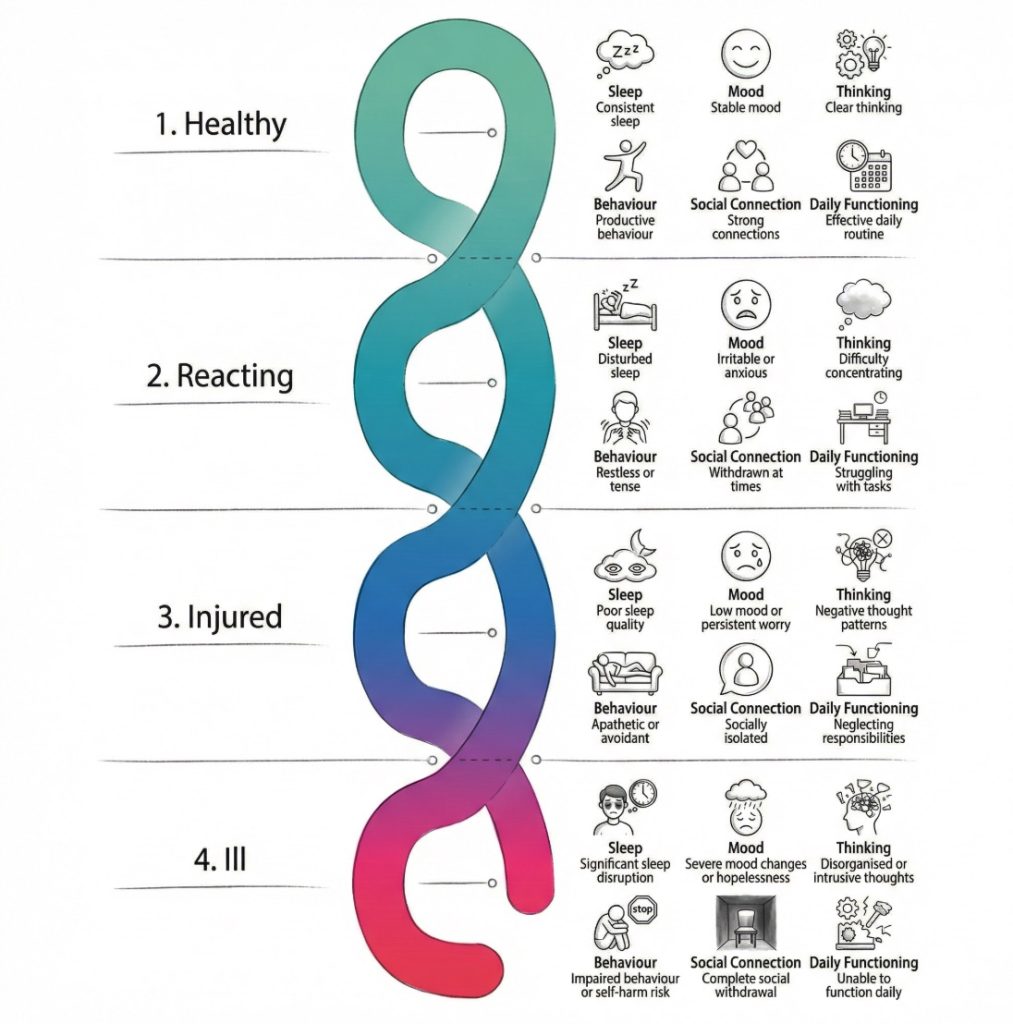
A few practical benefits stand out:
- Early signs: Small changes in sleep, appetite, mood, or behaviour can be noticed before distress becomes severe.
- Shared language: Teams, families, and professionals can describe change in a more consistent way.
- Less stigma: The language feels less fixed and less judgemental than blunt labels.
- Better records: Staff can describe what they see rather than guessing at diagnosis.
- Recovery focus: The model leaves room for improvement, relapse, and fluctuation.
A caveat here is that the continuum should not be treated as a strict scoring tool. People do not move through the stages in neat steps. They may improve in one area while struggling in another. They may also move quickly after a sudden event.
Still, the model remains useful because it keeps attention on what can actually be seen. The Care Quality Commission guidance on mental health services reflects that wider focus on safe care, rights, and the lived experience of people using services.
What the healthy stage looks like
The healthy stage means the person is coping well overall. Life may still be busy or stressful, but daily pressures are manageable. They can usually think clearly, recover after setbacks, maintain relationships, and keep up with ordinary routines.
Healthy does not mean cheerful all the time. It does not mean perfect sleep, constant productivity, or the absence of sadness and worry. It means the person has enough stability, coping capacity, and support to deal with normal ups and downs without losing their footing.
Common signs in the healthy stage include:
- Steady mood: Emotions rise and fall, but they do not dominate the day.
- Usual sleep: Sleep is settled enough to restore energy.
- Clear thinking: Concentration and decision making are broadly normal.
- Stable routine: Work, study, meals, relationships, and self care stay on track.
- Useful coping: The person uses habits that help, such as rest, exercise, routine, or talking to others.
The healthy stage looks different from one person to another. One person may thrive on a busy social life. Another may stay well through a quiet routine and limited demands. What counts is whether the person is functioning in a steady way for them.
Examples help to make this concrete:
- At home: A parent feels tired after a demanding week but still manages the household, keeps perspective, and makes time to recover.
- At work: A nurse handles pressure on a difficult shift, communicates clearly, and settles again after work.
- At college: A student feels nervous before exams but continues attending classes, sleeping reasonably well, and staying connected to friends.
- In a care home: A resident takes part in usual activities, follows their routine, and responds to others in their normal way.
This stage is also where baseline becomes important. Staff and families are often better placed to spot later change when they know what the person is like when they are settled. That links closely to person centred care under Regulation 9, where care should reflect the person’s needs and preferences.
“Healthy does not mean perfect. It means stable enough to cope.”
What the reacting stage means
The reacting stage is the early stage of strain. The person is still functioning, yet pressure is starting to show. Sleep may become lighter, concentration may dip, and ordinary frustrations may feel harder to handle. They are no longer quite at their usual baseline.
This stage often appears after stress builds up over days or weeks. A person may be juggling long shifts, caring for a relative, dealing with conflict at home, or carrying grief they have not had room to process. Meanwhile, they may still look outwardly capable. That is why reacting is easy to miss.
Typical signs in the reacting stage include:
- Poorer sleep: The person may wake more often or struggle to switch off at night.
- Irritability: Small setbacks may trigger sharper reactions than usual.
- Persistent worry: The mind stays busy, tense, or stuck on one problem.
- Reduced concentration: Reading, planning, or remembering small tasks may feel harder.
- Lower patience: Noise, change, pressure, or interruption may feel more difficult to tolerate.
- Mild withdrawal: The person may cancel plans or speak less than usual.
A realistic workplace example might involve a support worker who is still turning up and doing their job but has become short tempered, forgetful, and unusually quiet in handover. At home, reacting may show up as poor sleep, less appetite, or a growing reluctance to answer calls. In supported living, a person may become more unsettled in the evening, less engaged with activities, or more anxious about small changes in routine.
The reacting stage is often reversible. Rest, practical support, a lighter workload, honest conversation, and predictable routine may help a person move back towards healthy. Yet if those pressures continue unchecked, the person may slide further along the continuum.
A useful summary table makes the difference clearer:
| Stage | Usual picture | Day to day impact |
|---|---|---|
| Healthy | Stable mood, clear thinking, settled routine | Daily life feels manageable |
| Reacting | Worry, irritability, poor sleep, lower focus | Daily life continues, but with more effort |
| Injured | Persistent distress, withdrawal, decline in coping | Daily life is clearly affected |
| Ill | Severe symptoms, major risk, loss of function | Daily life may break down |
“Reacting is often the point where early help can change the direction.”
How the injured stage differs from reacting
The injured stage is more serious than reacting because the signs are stronger, longer lasting, and harder to shake off. Distress is no longer sitting at the edges of daily life. It is starting to shape the day.
The person may feel more anxious, more low, more numb, or more overwhelmed. Sleep problems may continue for weeks. Social contact may shrink. Motivation may drop away. Their usual coping habits no longer seem to be enough.
Common signs in the injured stage include:
- Ongoing sleep problems: Poor sleep continues and affects energy, patience, and focus during the day.
- Marked withdrawal: The person pulls back from people, work, study, or activities they would normally manage.
- Lower performance: Mistakes increase, tasks are missed, or basic routines begin to slip.
- Stronger distress: Tearfulness, panic, anger, hopelessness, or emotional flatness becomes more frequent.
- Physical effects: Headaches, exhaustion, loss of appetite, stomach problems, or muscle tension may become more obvious.
- Unhelpful coping: Alcohol use may rise, self neglect may appear, or the person may stay constantly busy to avoid difficult feelings.
A care worker might notice this stage in a resident who now avoids communal spaces, refuses personal care most mornings, and says they cannot face the day. At work, a previously reliable colleague may become tearful, absent more often, and unable to organise simple tasks. In education, a student may miss deadlines, stop attending, and pull away from friends.
There is sometimes a counter point here. People can go through a short intense period of stress, show several of these signs, and recover quickly once the stress passes. That is true. Yet the injured stage is usually marked by a clearer pattern of disruption over time, not just one difficult week.
The difference between reacting and injured comes down to three things:
- Duration: The problem lasts longer and keeps returning.
- Intensity: The signs are stronger and harder to hide.
- Impact: Work, self care, relationships, or safety begin to suffer.
The distinction helps people decide when ordinary support may no longer be enough. Skills for Care and the NHS mental health services pages both point to the value of recognising change early and linking people to the right level of support.
“Injured means the strain is no longer passing through. It is settling in.”
What the ill stage can look like
The ill stage sits at the far end of the continuum. Symptoms are severe, persistent, crisis level, or all three. The person’s usual coping methods are no longer enough. Daily functioning may be badly affected, and risk may increase.
This stage can look very different from one person to another. One person may be deeply depressed and unable to get out of bed, wash, or eat properly. Another may be in a state of panic and unable to leave the house. Another may become confused, paranoid, or detached from reality. Quiet collapse is still collapse.
Common signs in the ill stage include:
- Severe loss of function: The person cannot manage ordinary tasks safely or reliably.
- Intense distress: Anxiety, panic, despair, or agitation feels overwhelming.
- Risk concerns: There may be self harm, suicidal thinking, self neglect, or behaviour that places the person or others at risk.
- Disrupted thinking: Thoughts may become chaotic, very slowed, hopeless, or out of touch with reality.
- Near total withdrawal: The person may stop engaging with other people almost completely.
- Need for urgent support: Specialist mental health input, crisis care, or emergency services may be needed.
This is the stage where legal and professional frameworks may become especially relevant. The Mental Health Act 1983 governs certain aspects of assessment, care, and treatment for mental disorder. The Mental Capacity Act 2005 applies when there is doubt about whether a person can make a specific decision at the time it needs to be made. These are separate frameworks and they serve different purposes.
The NHS urgent mental health support pages and CQC information on mental health services show how safety, treatment, rights, and service quality come together when distress becomes severe.
How the continuum can be used day to day
The continuum works best when it is used as a practical guide rather than a rigid checklist. First, people need to know the person’s baseline. Next, they need to notice what has changed. After that, they need to look at how long the change has lasted and what effect it is having.
A simple step by step guide helps:
- Step 1: Know the baseline. Learn what the person is like when they are coping well.
- Step 2: Notice change. Look for what is new, stronger, or out of character.
- Step 3: Check duration. A difficult day is not the same as a difficult month.
- Step 4: Look at impact. Ask what is happening to sleep, work, self care, relationships, and safety.
- Step 5: Record clearly. Write what can be observed rather than labels or assumptions.
- Step 6: Share concerns. Pass on changes through the right channels in work or care settings.
- Step 7: Review again. Mental health may improve, worsen, or fluctuate.
This approach is useful across settings. A domiciliary care worker may notice that a person who is usually chatty has become withdrawn, is sleeping late, and has left meals untouched for several days. A school or college tutor may spot falling attendance, poor concentration, and withdrawal from friends. A manager may notice rising absence, irritability, and reduced performance in a member of staff.
The continuum also works well when people look at the same five areas each time:
- Mood: Has the person become more low, anxious, angry, or flat?
- Thinking: Are memory, concentration, and decision making still as usual?
- Behaviour: Are routines, communication, and habits changing?
- Physical signs: What is happening with sleep, appetite, tension, or energy?
- Functioning: Can the person still manage work, study, self care, and relationships?
This kind of observation supports the wider standards expected in regulated care. The fundamental standards enforced by CQC are built around safe care, person centred care, dignity, and protection from harm.
“The continuum is most useful when it changes what people notice.”
Where the continuum fits with roles, standards, and law
The continuum is a learning model, not a legal test. Still, it sits comfortably alongside existing duties in health and social care because it encourages careful observation, earlier response, and person centred support.
Several roles may be involved when a person moves along the continuum:
- GPs: Often the first professional contact when mental health begins to deteriorate.
- Mental health nurses: Assess, monitor, and support people in hospital and community settings.
- Psychiatrists: Provide specialist medical assessment and treatment planning.
- Social workers: Support care planning, safeguarding, rights, and access to services.
- Approved Mental Health Professionals: Coordinate certain Mental Health Act assessments.
- Care workers and support workers: Often notice the earliest changes in daily functioning.
- Registered managers: Oversee recording, escalation, staffing, and service response.
This link between observation and action is one of the strongest features of the continuum. A support worker may notice movement from reacting into injured. A GP or mental health practitioner may then assess the person in more depth. A manager may decide whether risk procedures or referral pathways need to be used.
Relevant standards and frameworks include:
- Mental Health Act 1983: Covers certain powers and duties linked to mental health assessment, care, and treatment.
- Mental Capacity Act 2005: Covers decision making where capacity is in doubt for a specific decision.
- Health and Social Care Act framework: Supports regulation of providers and service quality.
- Regulation 9: Sets out the requirement for person centred care.
- NICE guidance: Supports evidence based approaches to mental wellbeing and service quality.
- Skills for Care resources: Support workforce learning around mental health and wellbeing.
These links do not turn the continuum into a legal model. They show why it fits naturally with safe, observant, person centred care.
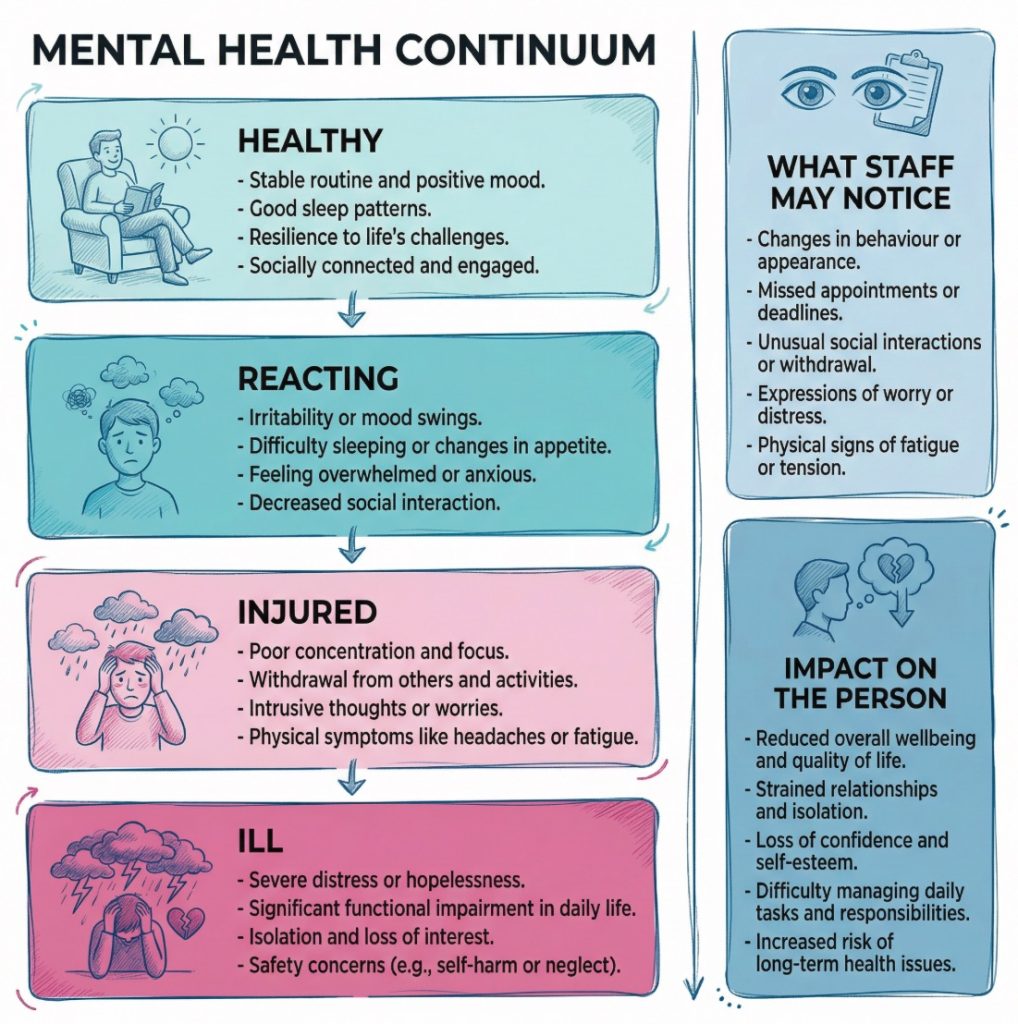
What common mistakes look like
The model is simple, but it can still be used badly. One common mistake is treating the stages as fixed labels. People do not move through them in neat order, and they do not stay in one stage forever. Another mistake is assuming that visible distress is the only sign that something is wrong.
People show strain in different ways. One person becomes tearful. Another becomes angry. Another grows quiet, detached, and hard to reach. Because of that, careful observation is more useful than assumptions.
Common mistakes include:
- Jumping to diagnosis: The continuum helps describe change, but it does not diagnose a condition.
- Ignoring baseline: Without knowing what is usual for the person, change is harder to judge.
- Focusing on one sign: A single symptom rarely tells the full story on its own.
- Using judgemental labels: Words such as lazy, manipulative, or difficult can hide what is really going on.
- Waiting too long: Small changes can turn into serious deterioration when nobody responds.
- Forgetting physical causes: Pain, infection, medication effects, menopause, and fatigue can all affect mental state.
- Mixing up legal frameworks: The Mental Health Act and the Mental Capacity Act do different jobs.
A short checklist helps keep the model grounded:
- Notice patterns: Look for more than one change at a time.
- Check impact: Ask what the change is doing to daily life.
- Record facts: Write what happened, when it happened, and how often.
- Compare with baseline: Decide whether this is usual or out of character.
- Think about safety: Consider risk, vulnerability, and deterioration.
- Use the right route: Share concerns through the correct service or management pathway.
Conclusion and next step
The four stages of the mental health continuum are healthy, reacting, injured, and ill. Together, they show that mental health can shift over time and that those shifts often appear before a crisis becomes obvious.
This model is useful because it connects everyday observation with clearer action. It helps families, staff, managers, and professionals describe change in a practical way. It also keeps the focus on the person rather than on blunt labels.
The clearest next step is simple. Notice change early, look at the effect on daily life, and place that change in context. That keeps the continuum grounded in real situations, where it is most useful.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.
