
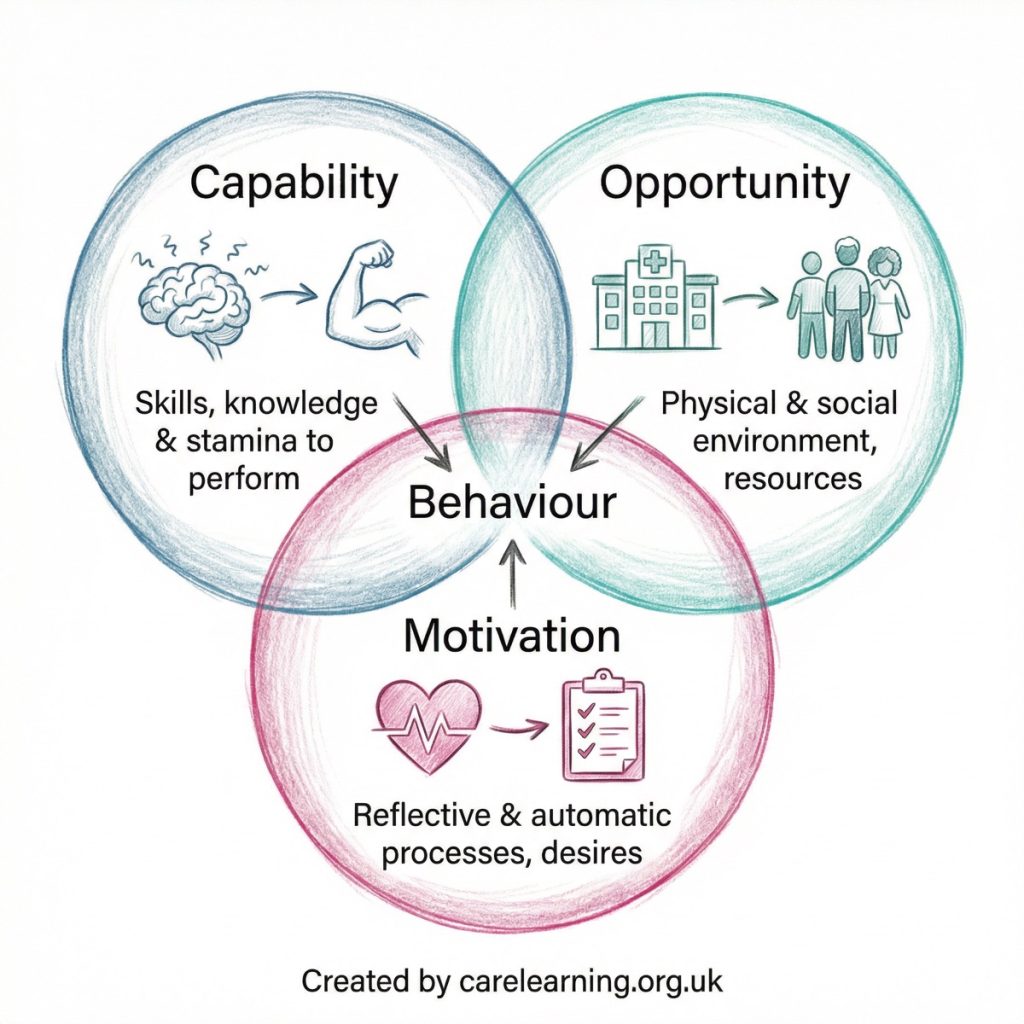
The COM-B model is a framework used to understand behaviour in the context of health and social care. It helps professionals work out why a person behaves in a certain way and what needs to change for desired behaviours to occur. COM-B stands for Capability, Opportunity, Motivation – Behaviour. The model is widely applied in assessing and influencing behaviours linked to health outcomes, treatment adherence, lifestyle changes, and everyday care decisions. It provides a clear structure for identifying barriers and supports that influence whether a behaviour happens or not.
The idea behind COM-B is simple but powerful: for any behaviour to take place, the individual must have the capability to do it, the opportunity to perform it, and the motivation to carry it out. All three elements interact with each other, influencing behaviour in both direct and indirect ways.
This approach is commonly applied when looking at changes such as improved medication routines, better diet, physical activity, or safer care practices. By breaking behaviour down into these elements, professionals can pinpoint what exactly needs attention and develop interventions accordingly.
What is Capability?
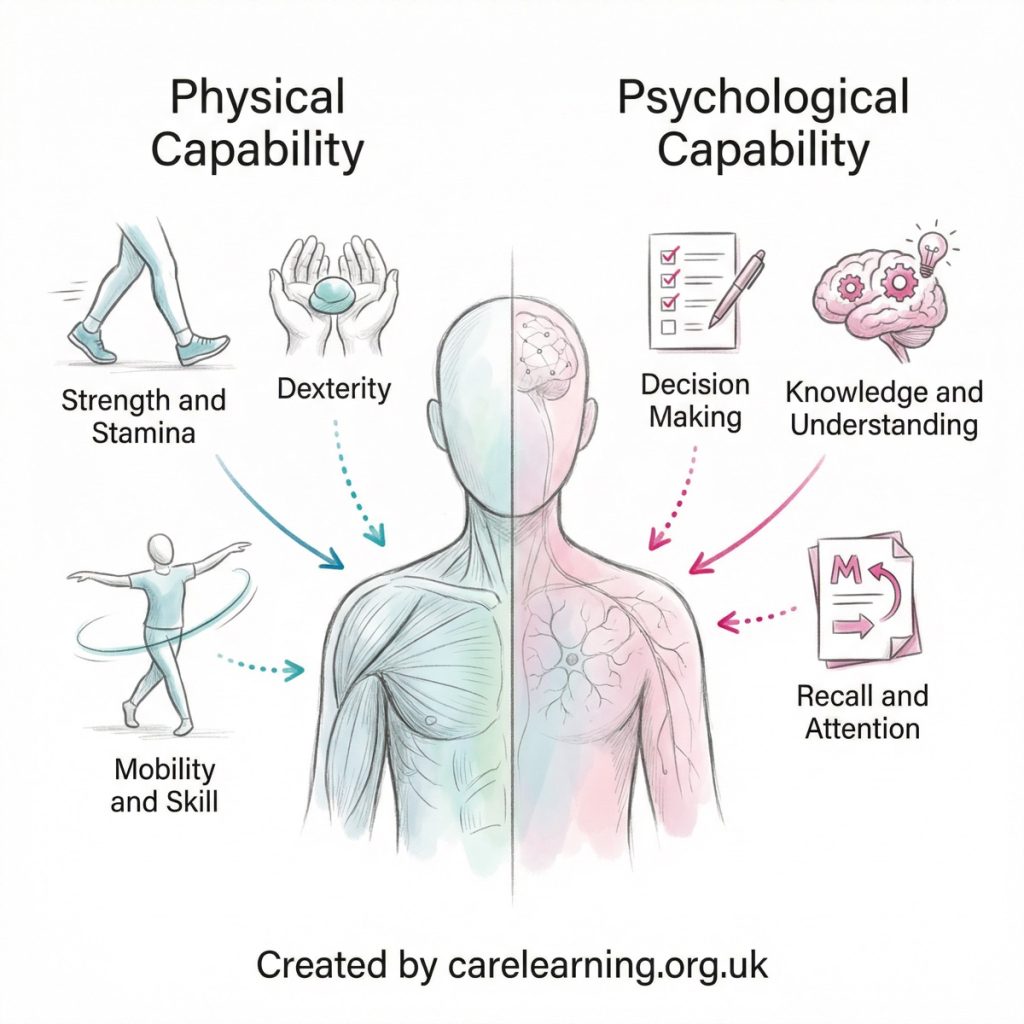
Capability refers to the person’s ability to perform a behaviour. This includes both physical capability and psychological capability.
Physical capability covers the physical skills, strength, stamina, or dexterity needed to perform the behaviour. For example, if a care plan requires a person to walk daily, they must have adequate mobility and physical strength to do so.
Psychological capability relates to the knowledge, awareness, and mental skills required. This could be understanding how to take medication correctly, being able to recognise symptoms, or having problem-solving skills. Without the mental ability to understand or remember the behaviour, it cannot be performed effectively.
Barriers to capability may include memory loss, physical disabilities, lack of training, and fatigue. Strengthening capability often involves education, skill-building exercises, assistive devices, or physiotherapy programmes.
Examples include:
- A patient learning how to measure their blood sugar levels accurately
- Training care staff to use specialised equipment safely
- Supporting a person with cognitive impairment using memory aids
Capability changes are often achieved through teaching, practice, and providing tools that make performance possible.
What is Opportunity?
Opportunity is about the factors outside the individual that make the behaviour possible or prompt it. Opportunity is divided into physical opportunity and social opportunity.
Physical opportunity refers to having the right environment, resources, and conditions in place. This could mean having access to suitable facilities, equipment, or safe spaces. In a care setting, it may involve having medication located conveniently or having transport to attend appointments.
Social opportunity involves the influence of social cues, cultural norms, and interactions with others. Encouragement from peers, family support, or cultural acceptance of certain behaviours all count as social opportunities. Social opportunity often affects motivation as well, because feeling supported can inspire individuals to act.
Without opportunity, even the most capable and motivated person may fail to carry out a behaviour. For example, a care worker may know how to record patient notes correctly, but without access to the correct forms or software, the behaviour cannot occur.
Examples of opportunity-building actions include:
- Providing wheelchair-accessible pathways in a care home
- Scheduling regular community exercise classes
- Creating support groups for people with chronic conditions
- Ensuring necessary tools and resources are in place for staff
Opportunity often requires organisational or environmental change, making it an area that professionals must address systematically.
What is Motivation?
Motivation refers to the processes that direct and sustain behaviour. It has two main types: reflective motivation and automatic motivation.
Reflective motivation involves conscious decision-making, planning, and evaluation of outcomes. For example, a person might decide to eat healthier after thinking about long-term health benefits.
Automatic motivation is influenced by emotions, impulses, habits, and responses that occur without deliberate thought. A person might instinctively avoid certain activities if they are associated with fear or unpleasant memories.
Motivation determines whether the individual initiates the behaviour and continues it over time. This means even with high capability and opportunity, low motivation will block sustained behavioural change.
Motivation can be encouraged by:
- Setting achievable goals
- Using positive reinforcement
- Creating habits through repetition
- Linking behaviour to personal values or emotional drivers
Barriers to motivation may come from low confidence, lack of interest, negative past experiences, anxiety, or competing priorities.
The Interaction between the Components
The COM-B model highlights the fact that capability, opportunity, and motivation influence each other. Improving capability alone might not lead to change if opportunity is lacking. Boosting opportunity without motivation will still leave behaviour unchanged. Addressing motivation without capability may cause frustration or failure.
For example, if a patient wants to improve fitness (motivation) and has a safe place to exercise (opportunity) but lacks physical stamina (capability), the behaviour may still fail. Conversely, someone might have the ability and resources but lacks the will to act.
In practice, professionals often assess all three elements together to create well-rounded interventions. They may use questionnaires, interviews, observations, or structured assessments to map out where barriers and supports exist.
Applying COM-B in Health and Social Care
COM-B is used widely in behaviour change programmes, care planning, patient support, and staff training. It helps ensure interventions are targeted effectively rather than applied in a one-size-fits-all manner. For example, in designing programmes to help patients quit smoking, professionals may:
- Strengthen capability by educating about withdrawal symptoms and coping strategies
- Increase opportunity by providing smoke-free environments and support groups
- Boost motivation through goal setting, messaging about benefits, and rewards
In medication adherence programmes, COM-B might be applied by:
- Providing training to improve understanding of dosage instructions (capability)
- Making medications available and easy to access (opportunity)
- Encouraging commitment through personal health goals and emotional support (motivation)
The model is flexible enough to apply to both individual patient behaviours and staff behaviours within healthcare organisations.
Benefits of Using the Model
Using COM-B can lead to:
- Clear identification of specific barriers to behaviour
- Better targeted interventions
- Improved collaboration between care teams
- Greater likelihood of sustainable behaviour change
- A structured approach that supports evaluation of outcomes
By breaking behaviour into its three component parts, it becomes easier to see where small changes can make a big difference.
Limitations to Keep in Mind
The COM-B model is a useful tool, but it is not a complete solution on its own. It is a framework designed to support analysis and planning, not a one-size-fits-all method. To be effective, it needs accurate information about the person, their environment, and their circumstances. Poor assessment can lead to inaccurate conclusions.
Some behaviours may be influenced by factors outside the COM-B framework, such as broader societal pressures, economic stability, or legal restrictions. In such cases, COM-B can still be part of the process but must be supported by other tools and approaches.
Practical Steps for Using COM-B
Applying the model often involves the following:
- Identifying the specific behaviour to be changed
- Analysing each component: capability, opportunity, motivation
- Determining which component is most lacking
- Designing targeted interventions for each component as needed
- Testing and monitoring changes
- Adjusting interventions based on feedback and progress
These steps can be repeated over time to maintain and improve results.
Final Thoughts
The COM-B model offers a clear, practical way to understand why behaviours occur or fail to occur. By breaking down behaviour into capability, opportunity, and motivation, it allows health and social care practitioners to focus their efforts where they will have the most effect. It encourages a balanced view where multiple factors are assessed together rather than in isolation.
Most importantly, COM-B can be applied to both individuals and teams, supporting efforts to improve patient outcomes and workplace practices alike. It is simple in concept but powerful in application, helping shape realistic strategies to bring about positive behavioural change.
Applying Knowledge and Examples
- Identify the barrier: Consider whether the difficulty relates to capability (skills/knowledge), opportunity (environment/support), or motivation (beliefs/emotions), based on observations and the person’s views.
- Tailor support within role: Use clear prompts, accessible information, and supportive routines; suggest reasonable adjustments through the right channels rather than changing plans informally.
- Review and record: Note what helped or hindered and share appropriately with the team; update records so support remains consistent and person-led.
Responsibilities and Legislation
- Within competence: COM-B can inform everyday support planning, but it should not replace specialist assessment; complex concerns are usually managed via referral/escalation pathways.
- Person-led planning: Changes should match the person’s goals, preferences and agreed outcomes in the care plan, aligning with Regulation 9 requirements.
- Consent and capacity: Any plan should follow local consent processes and Mental Capacity Act 2005 principles if decision-making needs support.
- Record updates: Where COM-B informs support, documentation and reviews should follow organisational standards, including risk assessments and care-plan change control.
Essential Skills and Evidence
- Non-blaming perspective: Considers capability, opportunity, and motivation as factors affecting behaviour, avoiding assumptions about “non-compliance”.
- Identifying barriers safely: Notes practical, environmental, and communication barriers and shares them through appropriate channels to inform care planning.
- Supporting participation: Helps the person break goals into achievable steps that fit their routine, while respecting consent and right to decline.
- Reasonable adjustments: Uses accessible information, prompts, and supportive routines where agreed, ensuring adjustments are inclusive and proportionate.
- Documentation and continuity: Records agreed approaches and observations so support remains consistent across staff and services.
Develop and Reflection
- Balanced thinking: When change is difficult, do I consider capability, opportunity and motivation rather than blaming the person?
- Practical barriers: Am I noticing environmental or routine barriers that the team could adjust within agreed plans and policies?
- Choice and control: Do I support the person to set small, realistic steps that they genuinely choose?
- Team consistency: Is information recorded clearly so colleagues support the same approach?
- Development: Practise mapping day-to-day scenarios to COM-B in supervision, focusing on supportive prompts, respectful encouragement and accurate documentation—while staying within role boundaries.
Further Learning and References
- The behaviour change wheel: a new method for characterising and designing behaviour change interventions
Introduces COM-B (Capability, Opportunity, Motivation influencing Behaviour) and links it to intervention design, making it ideal for accurate definitions. - Delivering better oral health: Chapter 3 behaviour change
Shows COM-B used in an applied NHS context, illustrating how the model guides practical behaviour change conversations and techniques. - The behaviour change wheel (UCL Discovery)
Provides an academic record of the framework and paper details, useful for referencing COM-B’s origin and formal publication.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.






