
Values in health and social care are the beliefs and principles that shape how support is given, how decisions are made, and how people are treated from one moment to the next. They sit underneath everyday care. Policies, care plans, training and procedures all have their place, but values shape the human side of the work. They affect tone of voice, patience, honesty, fairness and whether someone feels seen as a person rather than a task.
Across guidance from bodies such as NHS values in action, SCIE dignity in care, NICE shared decision making guidance and Skills for Care values based recruitment, the same themes keep appearing. Dignity, respect, compassion, inclusion, quality and partnership with the person receiving support. Different services may use slightly different language, but the direction stays much the same.
“Values show up in small choices long before they appear in a policy or a care plan.”
Values answer a deeper question than “What should staff do?” They ask what care should feel like for the person receiving it. Washing, dressing, helping with meals and recording information all need to be done properly. Still, the way those tasks are done can leave someone feeling safe and reassured, or ignored and exposed. Person centred care grows from that difference. It focuses on the individual’s wishes, life history, strengths, routines and right to be involved.
This also explains why values are so often discussed during recruitment. Services do not only look for technical skill. They also look for empathy, respect, openness and a willingness to reflect. Skills can be taught and refreshed. Attitude is harder to build from scratch.
The core values seen across care settings
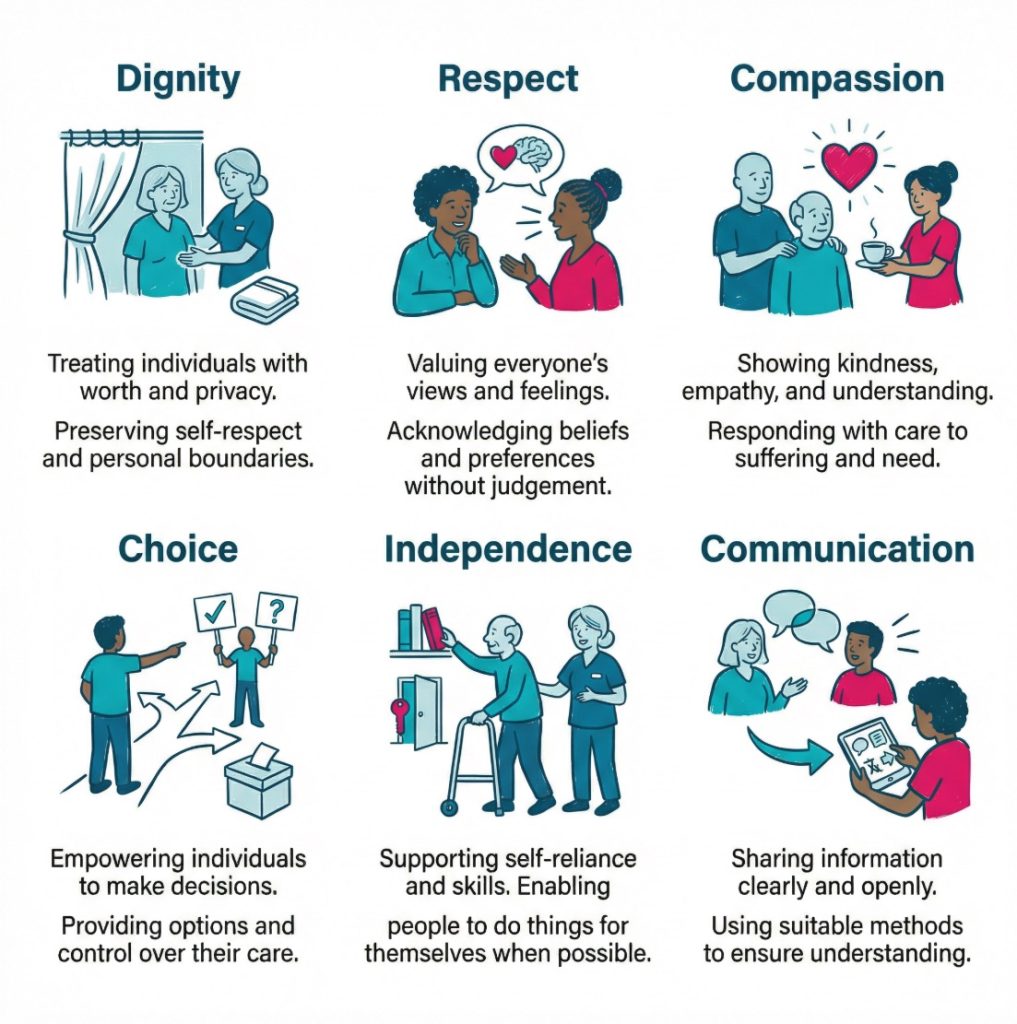
Most care settings talk about a similar group of values, even when the wording changes. Dignity means protecting a person’s self respect and not reducing them to a diagnosis, age group or care task. Respect means recognising the person’s identity, beliefs, preferences, culture, communication style and personal boundaries. Compassion means noticing distress and responding with warmth and humanity, not just efficiency.
Choice, independence, equality, inclusion, honesty and commitment to quality also sit near the centre of good care. Choice means involving people in decisions about their own support, including the ordinary decisions that shape daily life. Independence means helping people do what they can for themselves instead of taking over too quickly. Equality and inclusion mean care should not push someone to the edge because of disability, age, race, sex, religion, sexuality or language.
A common framework used in caring roles is the 6Cs. These are not the whole story, but they give a useful way to group the values staff are expected to show.
- Care: This keeps the person’s wellbeing at the centre of the work, not the convenience of the service.
- Compassion: This goes beyond politeness and includes empathy, kindness and emotional awareness.
- Competence: This means having the knowledge and skill to support people properly and knowing when to seek help.
- Communication: This covers clear, respectful communication with the individual, their family and the wider team.
- Courage: This includes speaking up when care is poor, unsafe or disrespectful.
- Commitment: This reflects reliability, professionalism and a steady focus on improving care.
Here is a simple comparison of how these values look in real settings:
| Value | What it looks like in care | Why it affects the person |
|---|---|---|
| Dignity | Knocking before entering, covering the person during personal care, speaking respectfully | The person feels safe, respected and less exposed |
| Respect | Using the right name, checking preferences, listening properly | The person feels recognised as an individual |
| Choice | Offering options about routines, meals, clothing or support | The person keeps more control over daily life |
| Independence | Encouraging the person to do what they can | Confidence and identity are more likely to be protected |
| Communication | Explaining clearly, checking understanding, noticing non verbal cues | Confusion reduces and trust often grows |
| Compassion | Responding kindly when someone is anxious or distressed | Emotional wellbeing is supported, not overlooked |
“People may forget the wording of a care plan, but they rarely forget how care made them feel.”
Taken together, these values shape not only what staff do, but how they do it. That difference can be felt straight away. Granted, routines have to run and records have to be completed. Yet people usually remember whether they felt respected, listened to and included.
How values shape day to day care
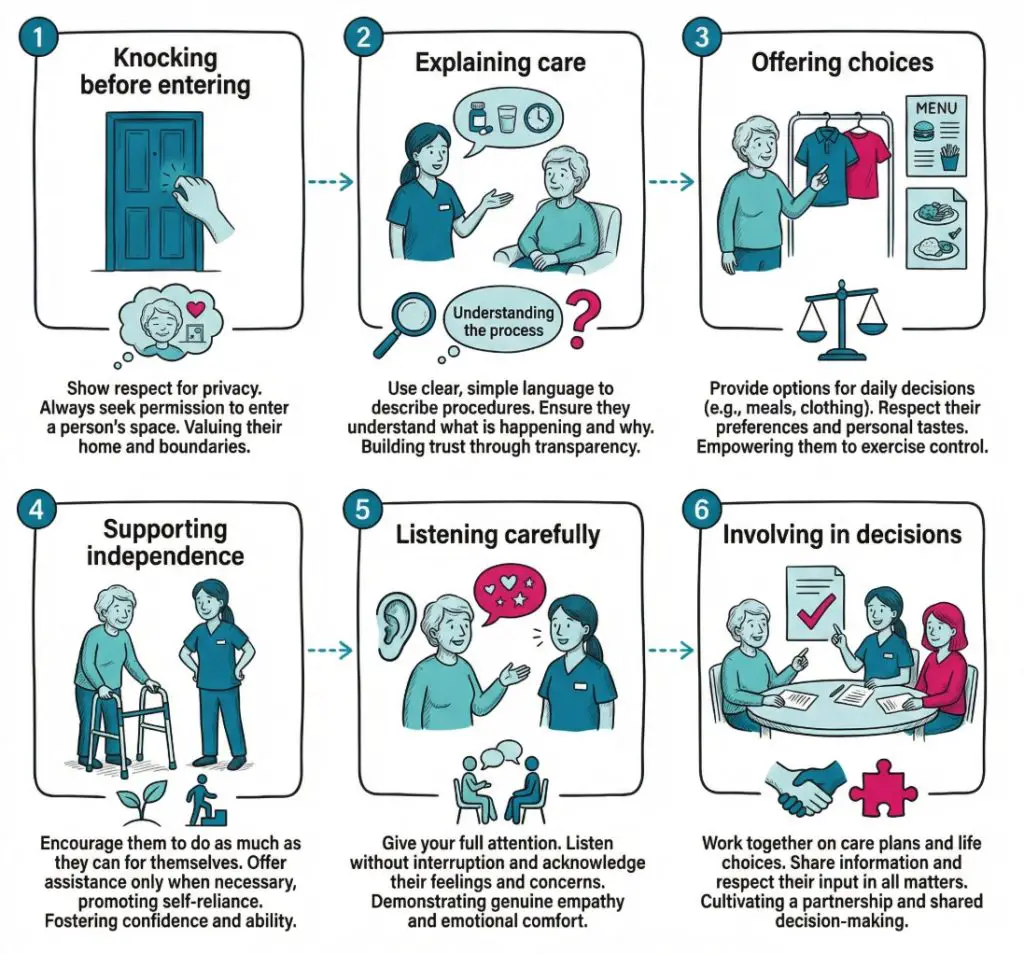
Values become visible in ordinary moments. A worker who values dignity knocks before entering a room, explains what they are doing and gives the person as much privacy as possible during personal care. A worker who values respect learns how the person likes to be addressed, checks routines instead of assuming and avoids talking over them. These are not grand gestures. They are daily habits.
Communication is one of the clearest examples. Good care is not only about passing on information. It includes listening, noticing body language, adapting language, checking whether someone has followed what was said and giving the person enough time to respond. This becomes especially important when someone lives with dementia, a learning disability, sensory loss, mental ill health or speech difficulties. Meanwhile, a rushed or careless approach can leave the person feeling confused or shut out.
Values also shape how staff balance safety and autonomy. Autonomy means a person’s ability to make choices about their own life. In care, this can be difficult. Staff may worry about risk and feel pressure to keep everything tightly controlled. A caveat here is that safety cannot be ignored. But a values based approach still asks what the person wants, what support could reduce the risk and how independence can be kept wherever possible.
For example, one person may want to make their own drink even if it takes longer. Another may want to choose their own clothes, walk to the garden alone or decide when to get up. Those choices may look small from the outside. For the person receiving care, they can shape identity, confidence and dignity.
- Privacy: Closing doors, drawing curtains and keeping conversations discreet can stop routine care from becoming intrusive.
- Choice: Offering real options, not token ones, helps the person stay involved in their own life.
- Listening: Paying attention to what the person says, or tries to say, can prevent distress and misunderstanding.
- Support for independence: Encouraging safe participation can protect confidence and reduce helplessness.
“Values are often most visible in the ordinary parts of the day.”
A counterpoint sometimes raised is that values sound idealistic when services are short staffed or under pressure. There is some truth in that. Busy settings can narrow people’s choices and compress conversations. On second thought, that is exactly why values need to stay in view. They help staff decide what should not be lost when time is tight.
Why values shape staff practice and service culture
For staff, values act as a guide when situations are busy, uncertain or emotionally demanding. Care work often involves competing demands, complex needs and moments where there is no perfect answer. Values help workers judge what good care should look like in that moment. They keep attention on the person’s dignity, voice and wellbeing, rather than on routine alone.
They also shape teamwork. Good care rarely depends on one worker acting alone. It usually relies on staff sharing information properly, respecting each other’s role and speaking up when something is wrong. A culture of openness can make it easier to raise concerns, reflect on mistakes and learn from feedback. Without that, poor habits can settle in and start to feel normal.
Skills for Care has placed strong emphasis on values based recruitment for this reason. Employers are not only asking whether a person can do the tasks required in the role. They are also asking whether that person’s behaviour and attitude fit the kind of care the service wants to deliver. You can see this in the Skills for Care overview of values based recruitment and the assessment tools for values based recruitment.
The wider service culture is shaped in the same way. Values should appear in recruitment, supervision, handovers, complaints handling, reflection and training. Not just on posters. Not just in mission statements. Where values are built into daily practice, people receiving care are more likely to feel that staff notice them as individuals. Staff are also more likely to feel able to challenge poor behaviour and support each other well.
A simple checklist can help show whether values are active in a service:
- Daily routines: Do routines fit the person, or does the person have to fit the routine.
- Communication: Do staff explain clearly, listen properly and check understanding.
- Privacy: Are personal conversations and personal care handled discreetly.
- Choice: Are people offered genuine options in daily life and care planning.
- Reflection: Do staff talk honestly about what went well and what needs to change.
- Speaking up: Do workers feel able to raise concerns without being shut down.
Even so, values do not remove every difficulty. They do give staff and organisations a reliable standard to return to when things become complicated.
What happens when values are missing
When values are missing, poor care does not always start with obvious abuse or clear neglect. It often begins with smaller patterns that become normal. Staff may talk about people within earshot as if they are objects of work. Personal care may be rushed. Privacy may be brushed aside because the service is busy. Choices may shrink because it is easier for staff to decide on the person’s behalf.
The result can be depersonalised care. Once that happens, it becomes easier to overlook distress, ignore preferences or justify care that suits the organisation more than the individual. For the person receiving support, the impact can be serious. Someone who feels humiliated during personal care may become anxious about asking for help again. Someone whose preferences are ignored may stop expressing them. Someone excluded from decisions may begin to feel powerless.
Poor values also affect communication. A person may not fully understand their options, may not feel able to ask questions or may agree to something simply because they do not feel included enough to say otherwise. That can damage trust. It can also make care feel like something being done to the person rather than with them.
For staff, weak values can create moral strain. This is the discomfort people feel when they know what good care should look like but work in conditions that make it harder to provide. Over time, that can affect morale, teamwork and staff retention. It can also reduce reflective practice because workers become focused on getting through the shift.
Common mistakes often sit at the centre of this problem:
- Rushing communication: Quick explanations can leave the person confused, anxious or silent.
- Assuming preferences: Staff may think they know what the person wants without checking.
- Taking over too soon: Support can slip into control when independence is not given enough weight.
- Using task led language: People can start to sound like workloads rather than individuals.
- Treating privacy as optional: Small lapses can quickly damage dignity and trust.
“When values slip, people often feel it before any report or complaint is written.”
A values based culture will not fix every pressure in care. Still, it creates a firmer base for humane and thoughtful support. It keeps bringing staff back to a simple question: what is this experience like for the person receiving care?
A practical way to look at values in care
It can help to think about values in three steps. First, look at the person. What do they prefer, what helps them feel safe and what routines or relationships are important to them. Second, look at the task. What has to be done, what risks are present and what support is needed. Third, look at the way the task is carried out. Is the person involved, informed and treated with respect throughout.
This approach is useful because it keeps care concrete. It stops values from becoming vague words on a training slide. It also links directly to staff responsibility. Workers are not only expected to complete tasks properly. They are expected to notice when the way support is being given could embarrass, exclude or disempower the person.
A short example shows how this works. An older adult needs help with washing and dressing in the morning. A task only approach focuses on getting this done quickly. A values based approach still gets the task done, but it also asks how the person prefers to start the day, what level of help they want, whether privacy is protected, whether choices are offered and whether their pace is being respected. Same task. Very different experience.
Another example could involve mealtimes. A task led service may deliver food at a fixed time and move on. A values led approach checks food preferences, communication needs, seating, dignity, pace and whether the person wants support or more independence. The practical care may look similar on paper. The lived experience often does not.
Useful takeaways from this topic include the following:
- Values are visible: They show up in tone, timing, privacy, choice and everyday behaviour.
- Small actions count: Knocking, listening and explaining can shape dignity as much as larger decisions.
- Culture affects care: Services that recruit, supervise and reflect through a values lens are more likely to deliver respectful support.
- Pressure tests values: Busy periods often reveal whether values are real or only written down.
- People feel the difference: Respectful care usually builds trust, while rushed care can quickly erode it.
Conclusion and next step
Values in health and social care are the guiding beliefs that shape behaviour, relationships and decisions. They turn care from a list of tasks into a human service built around dignity, respect, compassion, inclusion and quality. For individuals, these values can affect whether care feels safe, personal and empowering. For staff, they shape judgement, communication, teamwork and the confidence to speak up.
The clearest way to judge values is to look at daily care. Do staff listen. Do they protect privacy. Do they support choice. Do they speak respectfully. Do they see the person behind the need. Those questions often tell you more than any formal statement. For readers exploring the topic further, the SCIE page on privacy and dignity, the SCIE guide to communication and dignity, the NHS page on patient choice and the NICE page about shared decision making are all useful places to read next.
In the end, values are not abstract ideas. They can be seen in the small decisions that shape someone’s day, their confidence and sometimes their sense of self. That is why the subject stays so central in care.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.
