
A CQC observation visit is a visit where inspectors gather evidence by watching care, staff practice, and the care environment as support is delivered. Under the single assessment framework, observation sits alongside people’s experience, feedback from staff and leaders, feedback from partners, processes, and outcomes.
In adult social care, this gives inspectors a direct view of daily life. They can see how people are spoken to, how routines are carried out, how privacy is protected, and how well the service works when the day is moving at its usual pace. Records still count. Observation shows whether the written picture matches what people actually receive.
That is why these visits can feel more searching than a records check on its own. Good care is rarely proved by paperwork alone. It is seen in tone of voice, timing, patience, cleanliness, safe routines, and the way staff respond when someone needs reassurance or extra support.
“Observation shows the service people actually receive, not only the service described in records.”
The approach is especially relevant in care homes, supported living, and home care settings where inspectors can watch real interactions and compare them with care plans, risk assessments, audits, and feedback. A well-run service usually looks settled. People know what is happening. Staff know the person in front of them. The environment feels safe and lived in, rather than staged for the day.
Why observation visits carry so much weight
Observation visits carry weight because adult social care is practical and relational. Much of what people value most is visible in the ordinary parts of the day. A care plan may say that a person has choice, privacy, and support with independence. Observation shows whether that is true at breakfast, during personal care, on a medicine round, or when someone becomes distressed.
This connects closely with the fundamental standards and the Health and Social Care Act 2008 (Regulated Activities) Regulations 2014. Services are expected to deliver person-centred care, preserve dignity and respect, gain consent, provide safe care and treatment, protect people from abuse, and keep proper governance and staffing arrangements. Observation gives inspectors a clear way to test whether those duties are visible on the floor.
There is also a practical reason. Written systems can look neat while daily routines are rushed or inconsistent. A service may have a strong policy library and still show poor privacy, weak infection control, or task-led care. The reverse can happen too. A service with straightforward systems may deliver thoughtful, steady care that inspectors can see straight away.
One caution is worth keeping in view. A single visit only captures part of service life. That is true, but observation is not used on its own. It sits beside people’s experience, staff feedback, outcomes, and process evidence. Put together, those sources give a fuller picture than any one method alone.
What inspectors usually look for during an observation visit
Inspectors usually look for patterns rather than one polished moment. They notice how staff speak to people, whether language is respectful, whether people are given time to respond, and whether care is delivered at a pace that suits the person rather than the rota. Small things count. A knock on the door. A clear explanation before support begins. A quiet check that the person is happy to continue.
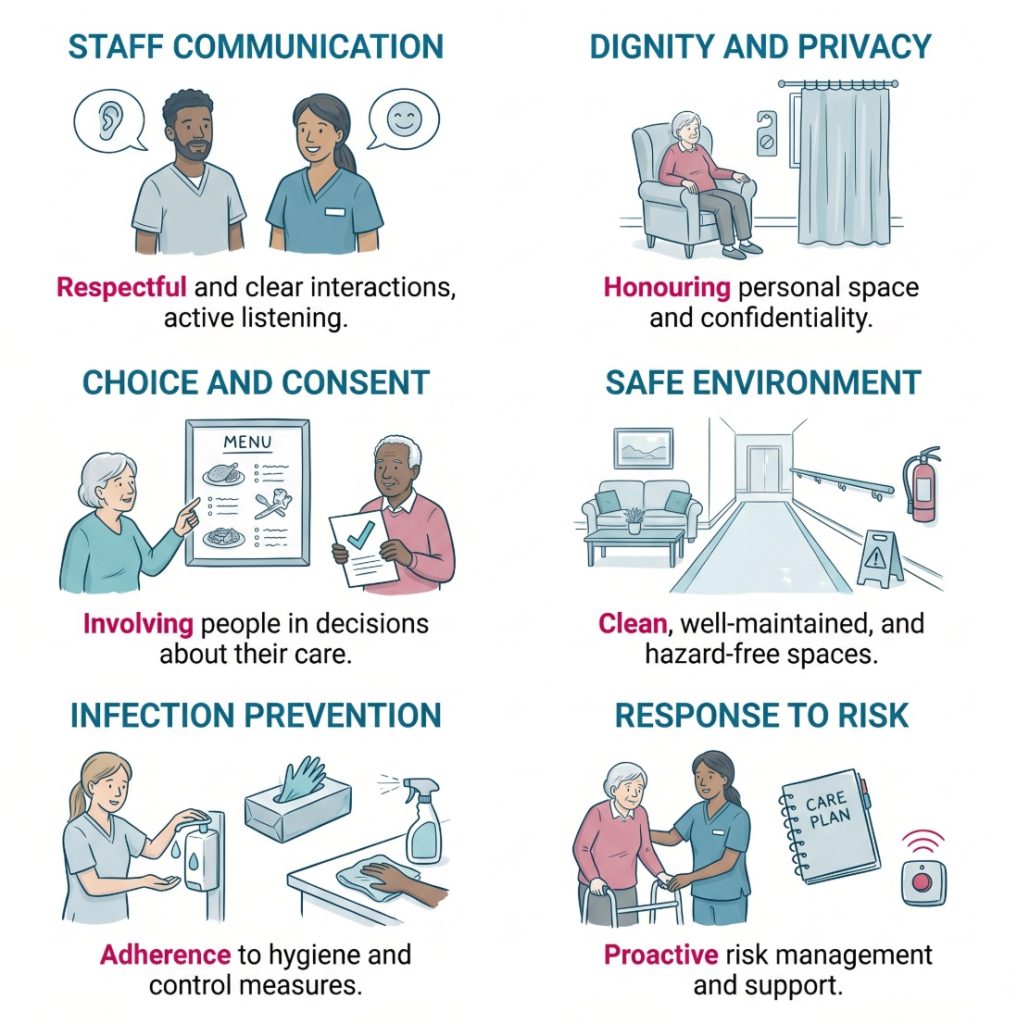
The CQC caring evidence categories for care homes and supported living link observation to staff practice, equipment, and the care environment. That covers kindness, dignity, treating people as individuals, independence, choice, control, and responding to immediate needs. Those themes are broad, but inspectors often see them in concrete details.
They may notice:
- Staff interaction: The tone of voice, patience shown, and whether staff listen properly. Respectful support often looks calm and unforced.
- Choice and consent: Whether people are offered real options and whether staff check agreement in a meaningful way. Consent is more than simple compliance.
- Independence: Whether staff help people do what they can still do for themselves. Support should not become taking over for the sake of speed.
- Privacy and dignity: Whether doors are closed, personal information is handled discreetly, and intimate care is carried out with care and sensitivity.
- Immediate response: Whether staff notice discomfort, distress, confusion, or fatigue and respond without delay.
- Safety and cleanliness: Whether the setting is uncluttered, hygienic, well maintained, and easy to move around.
“Inspectors rarely need a dramatic incident to judge a service. The ordinary routine usually tells the story.”
The environment speaks as clearly as the staff do. A clean dining room, accessible signage, safe equipment storage, and quiet private areas often suggest that daily oversight is strong. A cluttered corridor, poorly placed hoist, or careless conversation in a communal area can suggest the opposite.
How the legal and regulatory framework shapes observation
Observation visits sit within a legal and regulatory framework. The main body is the Care Quality Commission. The legal base includes the Health and Social Care Act 2008 (Regulated Activities) Regulations 2014, the Care Act 2014, the Mental Capacity Act 2005, the Human Rights Act 1998, and the Equality Act 2010.
Several regulations shape what inspectors may see during observation:
| What inspectors may see | Related regulation or framework | What it points to |
|---|---|---|
| Care built around the individual | Regulation 9 | Person-centred care |
| Privacy, respect, and tone | Regulation 10 | Dignity and respect |
| Real agreement and decision-making | Regulation 11 and the Mental Capacity Act 2005 | Consent |
| Safe routines, equipment, and risk controls | Regulation 12 | Safe care and treatment |
| Alertness to abuse, neglect, or poor practice | Regulation 13 and the Care Act 2014 | Safeguarding |
| Audit trails, action plans, and oversight | Regulation 17 | Good governance |
| Enough competent staff on shift | Regulation 18 | Staffing |
The legal background is important, but daily care should not sound like a legal briefing. Inspectors are not usually looking for staff to quote regulation numbers back to them. They look for services to work in ways that reflect those duties. A care worker who preserves privacy during personal care is showing Regulation 10 in action, whether or not they ever name it.
Communication belongs here as well. CQC includes providing information within its assessment approach, and this sits neatly with the Accessible Information Standard. If information is not accessible, choice, involvement, and consent can quickly become weak.
How to prepare the environment before an observation visit
The strongest preparation is routine, not theatre. Services that stay tidy, safe, and organised each day usually present well when inspectors arrive. Services that rely on a burst of last-minute activity often look tense. Records go missing. Equipment is shifted in a rush. Staff seem distracted.
A good environment is not about polish alone. It is about safety, dignity, and ease of use. Shared areas should be clean and comfortable. Corridors should be free from clutter. Bathrooms should be hygienic and stocked. Bedrooms should support privacy. Equipment should be available, checked, and stored safely. Signage should suit the people who live there, especially where dementia, sensory loss, or communication needs are part of daily care.
A simple sequence often helps keep standards steady:
- Walk-through checks: Senior staff can look at the service as a relative or visitor would see it. First impressions count.
- High-risk area review: Medicines rooms, sluices, bathrooms, kitchens, equipment stores, and entrances often reveal whether routines are sound.
- Accessibility check: Signs, written information, and layout should be clear enough for the people using the service.
- Privacy check: Conversations, handovers, and personal care spaces should protect dignity.
- Repair and replacement log: Worn furnishings, broken fittings, and unsafe equipment can point to weak oversight if left unresolved.
This ties in with day-to-day safety standards as well. The Health and Safety Executive expects care services to manage risk sensibly, and the same principle runs through observation visits. Safe moving and handling, sensible storage, and clear access routes are never just housekeeping points. They shape the safety of the whole shift.
A care home example brings this into view. One corridor regularly fills with linen bags during the morning round. Staff may see it as temporary. Inspectors may see reduced access, trip risk, and a sign that the service’s routine is shaping the building more than people’s safety.
“A service rarely looks prepared by chance. It usually looks prepared because daily routines are already well run.”
What documentation should be ready and why it supports observation
Observation does not replace documentation. It works alongside it. Inspectors often compare what they see with care plans, risk assessments, incident records, medicine records, training logs, complaints records, supervision notes, and audits. They are testing whether the paperwork is current, accurate, and reflected in practice.
Useful documentation is easy to find and easy to connect. If a person has had several falls, there should usually be an incident record, a reviewed risk assessment, an updated care plan, and evidence that staff were told about the changes. If a complaint was raised about delays, there should be some sign of review, action, and follow-up. This is where good governance becomes visible.
Records that commonly support observation include:
- Care plans: These should show the person’s needs, preferences, communication style, routines, and outcomes.
- Risk assessments: These should reflect current risks and show review, not just old concerns copied forward.
- MCA records: Where relevant, records linked to the Mental Capacity Act help show how decisions are approached lawfully.
- Medicines records: These can support what inspectors see on a medicine round and whether audits pick up concerns.
- Safeguarding records: These should show recognition, reporting, follow-up, and learning.
- Audits and action plans: These show whether leaders spot issues and act on them.
- Training and supervision records: These help show whether staff are supported to work safely and consistently.
NICE guidance on decision-making and mental capacity is useful here because it links legal duties to day-to-day practice. The same goes for SCIE’s Mental Capacity Act resource and SCIE’s safeguarding adults resources. Those sources do not replace local policy, but they help explain what good application looks like.
A supported living example makes the point well. One person misses doses when their usual worker is away. Observation may show a handover gap or a member of staff who seems unsure. If the records show that medicine audits picked up the pattern, the support plan was revised, and staff were briefed, the service looks engaged and responsive. If the paperwork sits silent, the concern grows.
How to help staff feel confident without sounding rehearsed
Staff confidence shapes what inspectors see. Nervous staff often become overly formal, forget to explain what they are doing, or fall back on stock phrases. The strongest preparation gives staff clarity about their role, the people they support, and the reasons behind their actions. It does not turn them into performers.
Good support can usually be explained in plain language. A sentence such as “He needs extra time in the morning because he is slow to process information before breakfast” is clear, practical, and grounded in the person’s needs. It says more than broad phrases about high-quality care.
You hear the same point from experienced workers again and again, usually in plain words. “If I rush him, I lose him for the rest of the morning.” That is not policy language. It is frontline judgement, and it often says more than a long checklist.
Useful staff preparation often includes:
- Short meeting discussions: One theme at a time, such as dignity, consent, or responding to distress, linked to real scenarios from the service.
- Observation by seniors: A medicine round, mealtime, or moving and handling task can be reviewed with feedback afterwards.
- Supervision with examples: Staff can talk through how they support one person’s choices, communication, and safety.
- Refresher learning: Core topics such as safeguarding, the Mental Capacity Act, infection prevention, and documentation stay alive when revisited regularly.
- Role clarity: Registered managers, deputies, seniors, and care staff each need to know their part in maintaining standards.
This section also links naturally with the Care Certificate standards and wider Skills for Care workforce guidance. Observation visits often expose weak induction, patchy supervision, or unclear expectations long before those problems show up in formal review.
A home care example shows how this works. A worker supporting a person with hearing loss speaks face to face, uses short clear sentences, and checks that the person has understood the plan for the visit. If asked why, the worker can explain that this reduces confusion and helps the person stay involved. That sounds natural because it is natural.
One brief caveat belongs here. Staff do not need perfect answers. They need honest and sensible ones. Guessing when unsure tends to create more concern than saying who can help.
What person-centred, rights-based care looks like on the day
Person-centred care is care built around the individual rather than the easiest routine for the service. Rights-based care means the person keeps their dignity, privacy, voice, relationships, identity, and control while receiving support. These ideas can sound broad on paper. During observation, they usually appear in small, ordinary actions.
A service shows this well when staff know what is important to the person. That may include the time they prefer to rise, how they like to be addressed, whether they want quiet before breakfast, how they communicate pain, what faith or cultural needs shape the day, and what support helps them stay as independent as possible.
Examples in different settings bring this into focus:
- Care home example: A resident living with dementia becomes anxious if rushed. Staff approach slowly, explain one step at a time, and allow the person to choose the order of washing and dressing.
- Supported living example: A person wants to go to the shops alone. Staff support safer planning rather than blocking the activity outright.
- Home care example: Visit timing reflects the person’s normal routine rather than the most convenient slot on the rota.
This sits comfortably with Skills for Care material on person-centred support and with broader NHS guidance on social care and support. It also sits alongside the Human Rights Act and Equality Act because fair treatment, privacy, identity, and reasonable adjustment run through everyday care.
You sometimes hear a carer sum it up more sharply than any training pack does: “She’ll tell you what she wants, but only if you slow down enough to notice.” That is a realistic picture of rights-based care. Not dramatic. Just observant.
“Person-centred care is often visible in the pause before action, not only in the action itself.”
A service can claim to offer choice while limiting what is actually possible. Real choice is usable choice. A person with hearing loss may need reduced background noise. A person with a learning disability may need pictures or extra time. A person with fluctuating capacity may need decisions approached at a better time of day. Those details decide whether rights are real or only described.
How safeguarding and risk management show up during observation
Safeguarding is not tucked away in a policy file. It appears in alert staff, careful handovers, accurate records, and confident reporting. Inspectors may notice whether staff pick up changes in mood, fear, injury, personal presentation, or interaction with others. They may also notice whether concerns are taken seriously or brushed aside.
The legal frame here includes Regulation 13 and the wider safeguarding duties linked to the Care Act 2014. Services should also be able to show how concerns are recognised, reported, escalated, and reviewed. A settled culture helps here. Staff who are used to raising concerns early tend to show more assurance when inspectors are present.
Risk management sits close to safeguarding, but it is not the same thing. Good risk management balances safety with autonomy. It does not remove every possible risk. That approach is often described as positive risk-taking. The phrase means that a person is supported to do what is important to them while sensible controls are put in place.
Examples help:
- Cooking in supported living: A person has left pans unattended before. Safer practice may involve prompts, a revised risk assessment, supervision at key points, and review.
- Walking independently in a care home: A resident wants to move about freely despite falls risk. A balanced response may use footwear checks, mobility aids, observation, and review rather than blanket restriction.
- Home care and medicines: A person wants to manage some medicines themselves. Support may include storage controls, prompts, and regular review rather than automatic removal of control.
The HSE guidance for social care is relevant here because it supports proportionate risk control rather than blanket avoidance. The same balance runs through good adult social care. People should be safe, but they should also be able to live.
Near misses belong in this picture as well. A near miss is an event that could have caused harm but did not. Services that record and review near misses often show stronger leadership because they learn before harm occurs.
Where feedback fits alongside observation
Observation gives a direct view. Feedback gives context. People’s experience remains one of the central evidence categories, and it helps inspectors judge whether what they see on the day reflects the usual experience of the service.
Feedback may come from people using the service, relatives, advocates, commissioners, visiting professionals, or staff. It may appear through complaints, compliments, surveys, review meetings, informal comments, or quality checks. The strongest services can show that they do more than collect it. They use it.
Useful signs include:
- Visible routes for concerns: People and families know how to raise worries or complaints.
- Trend review: Repeated issues are tracked rather than treated as isolated events.
- Action after feedback: The service can show what changed and whether the change worked.
- Open staff voice: Staff feedback is taken seriously because staff often spot pressure points early.
A care home may receive repeated family comments about poor updates after minor health changes. Observation might still show kind support. Both can be true. If leaders can show revised communication routines, supervision notes, and a check that relatives noticed the improvement, the service looks reflective rather than defensive.
How leaders and staff can respond during and after the visit
When inspectors arrive, the tone set by leaders often stays with the visit. A calm welcome, a concise overview of the service, and prompt access to key evidence usually help. Services do not need to create a special show. Normal care should continue as far as possible.
Staff responses are usually strongest when they are simple and direct. If an inspector asks what a worker is doing, the answer should describe the support and the reason for it. If something is not known, it is better to say so and point to the right person than to improvise.
After the visit, useful review points often include:
- What inspectors asked for: This shows which areas drew attention.
- What was easy to evidence: These are often strengths or areas with mature systems.
- What felt harder to explain: These points may highlight gaps in training, supervision, records, or oversight.
- What informal feedback was given: Early comments can feed into action planning before a formal outcome arrives.
- What needs to change: A clear action plan helps leaders turn observation into service improvement.
“A good response to inspection is not a performance on the day. It is steady follow-through afterwards.”
This is where governance earns its keep. If a service only reacts during inspection week, the same weaknesses often reappear. If leaders use the visit to refine systems, the service becomes stronger long after inspectors leave.
Common mistakes that weaken observation readiness
Several common mistakes recur across adult social care settings. The first is focusing too heavily on presentation and too lightly on daily care. A tidy reception area and a full inspection folder do not compensate for rushed support, poor privacy, or weak staff knowledge.
Another common problem is treating observation as separate from governance. It is not separate. Weak audits, poor follow-up, patchy supervision, and inconsistent handovers all show up in care sooner or later. Observation often exposes leadership gaps because daily routines reflect the systems behind them.
A third mistake is using vague language with staff. Broad messages such as “show good care” or “remember CQC” do not prepare teams properly. Staff need clear discussion about consent, dignity, communication, risk, safeguarding, and record keeping in their own setting with the people they support.
Common examples include:
- Over-tidying without fixing routine issues: The building looks better for a day, but the same unsafe habits remain.
- Old records left in place: Risk assessments and care plans stop matching what staff are actually doing.
- Staff who know the task but not the person: Support becomes mechanical and less respectful.
- Weak communication adjustments: People are spoken to, but not in a way they can truly follow.
- Delayed action after incidents: The event is recorded, but the service learns very little from it.
Small slips can alter the overall picture. Discussing a person in a corridor. Failing to notice discomfort. Leaving equipment in the wrong place. Missing a chance to offer choice. Piece by piece, these things shape how the service feels.
How to stay inspection-ready all year
The strongest services stay ready because their quality checks are woven into normal management. They do not rely on guessing when inspection may happen. They use regular walk-throughs, spot checks, supervision, audit cycles, feedback review, and peer observation to keep the service grounded in daily reality.
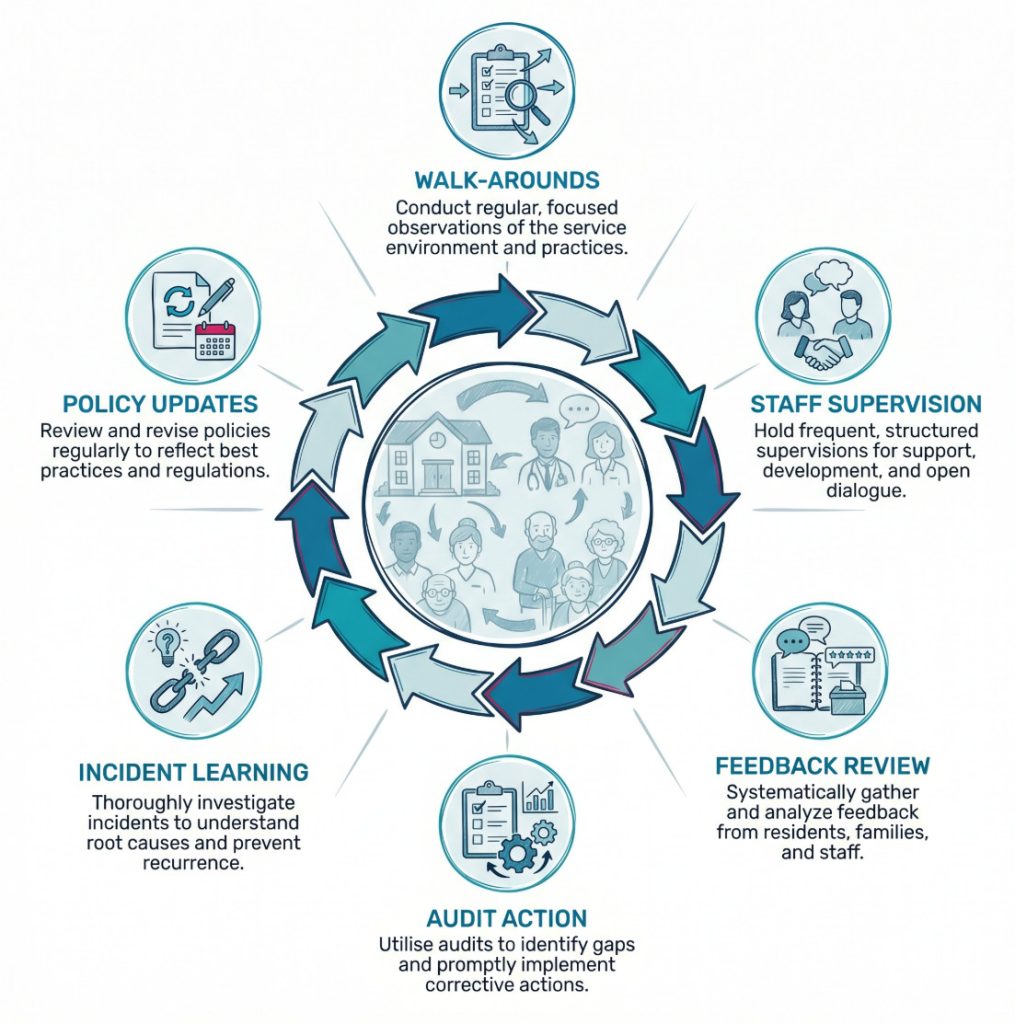
A practical year-round checklist often includes:
- Regular walk-rounds: Leaders look at the environment, routines, and interactions, not only the records.
- Practice observations: Mealtimes, medicines rounds, personal care, and handovers are watched and reviewed.
- Current records: Care plans, risk assessments, training records, and audits stay up to date.
- Feedback review: Complaints, compliments, surveys, and informal comments are tracked for patterns.
- Learning from incidents: Near misses, falls, safeguarding concerns, and medicine issues lead to review and action.
- Staff development: Supervision, competency checks, and refresher learning keep standards live.
- Involvement of people using the service: Their views feed into quality review rather than sitting apart from it.
This approach usually works better than a short burst of preparation. It is also more honest. A service that keeps asking whether people are treated with dignity, whether staff know the person well, whether risks are controlled sensibly, and whether records lead to action is usually in a stronger position when inspectors arrive.
Conclusion
CQC observation visits focus on what can be seen, heard, and experienced in the service itself. They test whether written systems reach real care. They show whether dignity, consent, safety, choice, safeguarding, and leadership are visible in ordinary routines.
Services usually come across best when the basics are strong every day. Staff know the people they support. Leaders watch practice as closely as paperwork. Risks are reviewed. Feedback leads to change. Records support care instead of standing in for it. Observation then becomes a fair reflection of the service rather than a day to get through.
The next step for any service is rarely dramatic. It is often a quieter piece of work. Daily walk-throughs. Better follow-up after incidents. Clearer staff discussion about consent and communication. More careful review of what people and families say. That is where observation readiness is built. Slowly. Properly.
Subscribe to Newsletter
Get the latest news and updates from Care Learning and be first to know about our free courses when they launch.
